Apr 9, 2026
Chronic joint and tendon pain can significantly impact your quality of life—limiting movement, reducing activity levels, and making even everyday tasks uncomfortable. While traditional treatments like medications, physical therapy, and surgery have long been the standard, regenerative medicine is transforming how we approach musculoskeletal injuries. One of the most promising advancements in this space is Platelet-Rich Plasma (PRP) therapy.
PRP therapy offers a minimally invasive, non-surgical option that uses your body’s natural healing mechanisms to repair damaged tissues. But what exactly is PRP, and how does it work? Let’s break it down.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses a concentrated form of your own blood to promote healing. Blood contains several components, including red blood cells, white blood cells, plasma, and platelets. Platelets are especially important because they contain growth factors and proteins that play a key role in tissue repair and regeneration.
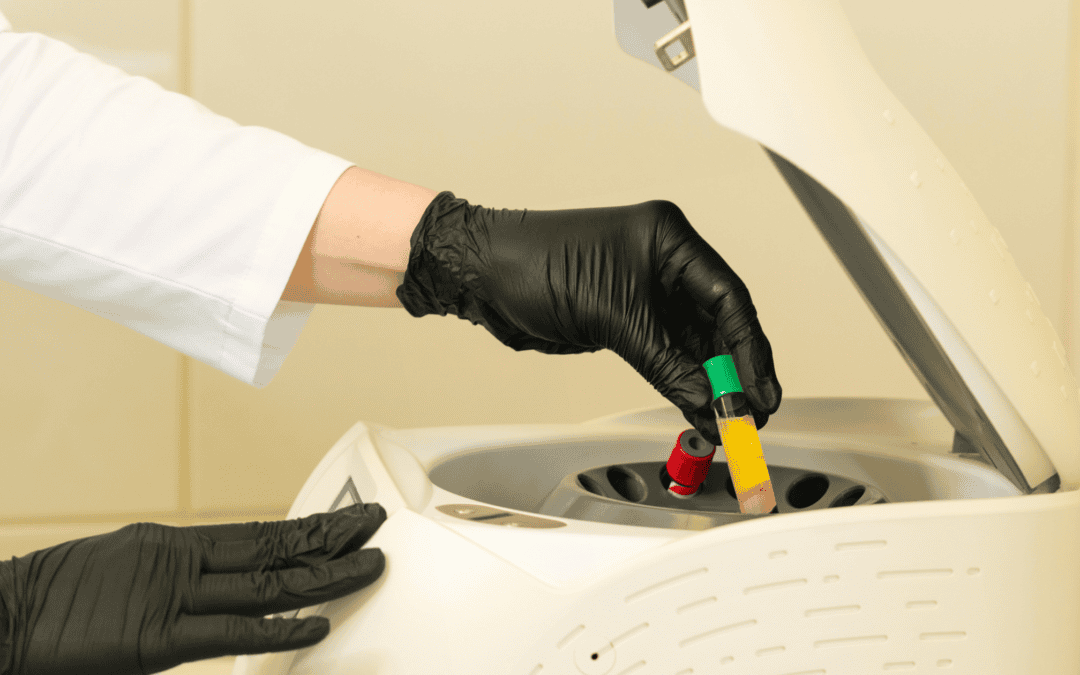
In PRP therapy, a small sample of your blood is drawn and placed in a centrifuge. This process separates the platelets from other blood components, creating a concentrated solution rich in healing factors. The PRP is then injected directly into the injured or painful area.
How PRP Promotes Healing
- Stimulates cell regeneration
- Promotes collagen production
- Improves blood flow to the injured area
- Reduces inflammation
- Accelerates tissue repair
Unlike corticosteroid injections, which primarily reduce inflammation temporarily, PRP targets the underlying cause of pain by supporting actual tissue healing.
Conditions PRP Can Treat
Joint Conditions
- Osteoarthritis (knee, hip, shoulder)
- Degenerative joint disease
- Cartilage injuries
Tendon Injuries
- Tennis elbow (lateral epicondylitis)
- Golfer’s elbow (medial epicondylitis)
- Achilles tendinitis
- Patellar tendinitis (jumper’s knee)
- Rotator cuff injuries
Ligament Injuries
- Partial ligament tears
- Chronic sprains
What to Expect During the Procedure
- Blood Draw: A small amount of blood is taken from your arm.
- Centrifugation: The blood is spun in a centrifuge to isolate the platelet-rich plasma.
- Injection: The PRP is injected into the targeted area, often using ultrasound guidance for precision.
Recovery and Results
One of the major advantages of PRP therapy is its relatively quick recovery time. Because it is a minimally invasive procedure, patients can often return to normal activities within a few days.
However, it’s important to note that PRP is not an instant fix. Since it works by stimulating natural healing, results develop gradually over time. Patients may begin to notice improvement within a few weeks, with continued progress over several months.
Benefits of PRP Therapy
- Minimally invasive
- Uses your body’s own cells
- Targets the root cause of pain
- Reduced downtime
- Versatile treatment option
Are You a Good Candidate for PRP?
PRP therapy is an excellent option for many patients, but it may not be suitable for everyone. Ideal candidates typically include individuals who have chronic joint or tendon pain, have not found relief with conservative treatments, and want to avoid or delay surgery.
PRP vs. Other Treatments
Corticosteroid injections provide short-term relief but do not promote healing. Physical therapy is beneficial but may not be enough for chronic conditions. Surgery can be effective but comes with higher risks and longer recovery times. PRP offers a regenerative alternative without the invasiveness of surgery.
Final Thoughts
If you’re struggling with persistent joint or tendon pain, PRP therapy may offer a safe, effective, and minimally invasive solution. By harnessing your body’s natural healing power, this innovative treatment helps restore function and improve quality of life.
At SDOMG, our team specializes in advanced, patient-centered treatments designed to help you get back to the activities you love. Schedule a consultation today to learn if PRP therapy is right for you.
Apr 14, 2025
Joint pain can be a daily struggle, affecting everything from simple walks to sleep and overall quality of life. For many, traditional treatments like physical therapy, medications, or even surgery provide only limited relief—or come with side effects and long recovery times. That’s where regenerative medicine steps in, offering innovative options like Platelet-Rich Plasma (PRP) and Cell Therapy. These treatments harness the body’s own healing powers to target the root of joint pain, not just mask the symptoms.
If you’re curious about how PRP and Cell Therapy work, and whether they might be right for you or someone you love, read on. We’ll break down the science in simple terms and explore how these therapies are changing the way we treat joint issues.
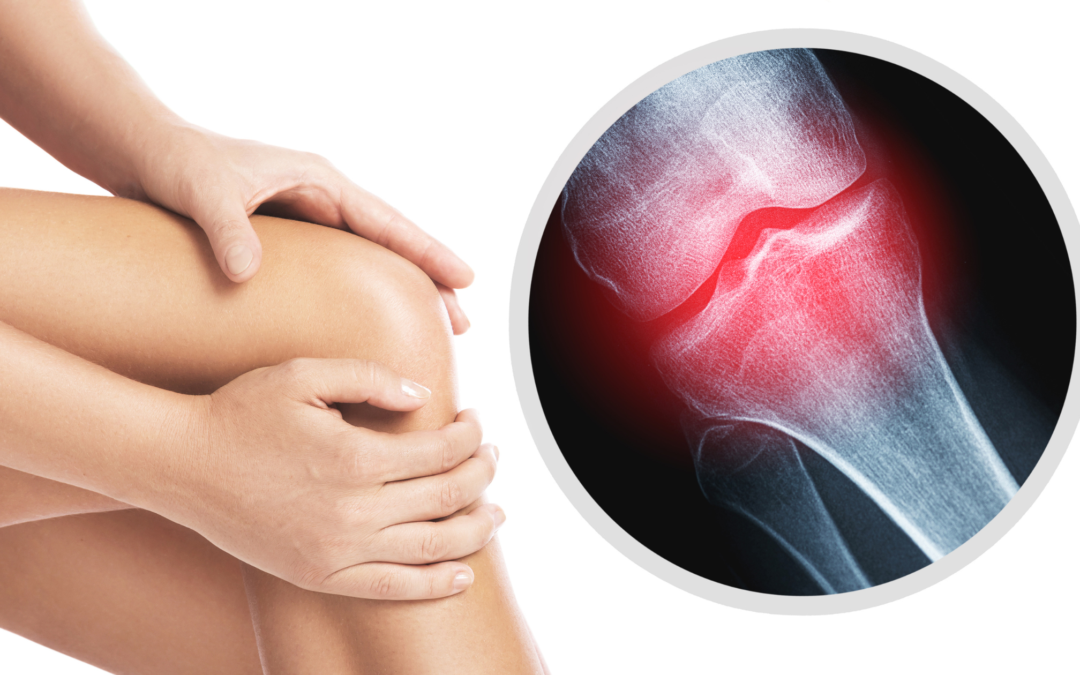
What Causes Joint Pain?
Joint pain can stem from many sources: injury, overuse, inflammation, arthritis (especially osteoarthritis), or even simple aging. The cartilage that cushions joints can wear down, tendons and ligaments can become inflamed or torn, and the surrounding tissues may degenerate over time.
Traditionally, options like corticosteroid injections or anti-inflammatory drugs have been used to reduce pain. However, these don’t actually repair damage—they just offer temporary relief. That’s where regenerative therapies like PRP and cell therapy stand apart: they aim to stimulate healing, not just dull the pain.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a treatment that uses a concentration of your own platelets to accelerate healing in damaged joints and tissues.
How It Works:
- Blood Draw: A small amount of your blood is drawn—similar to a standard lab test.
- Separation: The blood is spun in a centrifuge to separate the platelets from other components like red and white blood cells.
- Injection: The resulting platelet-rich plasma is injected directly into the affected joint.
Platelets are best known for clotting blood, but they also contain growth factors—powerful proteins that promote tissue repair, reduce inflammation, and stimulate cell regeneration. By injecting a high concentration of these growth factors directly into the joint, PRP therapy encourages the body to repair itself.
What It’s Used For:
- Osteoarthritis (knee, hip, shoulder)
- Tendonitis
- Ligament injuries
- Cartilage damage
- Sports injuries
What Is Cell Therapy?
Cell therapy—often referred to as stem cell therapy—uses the body’s own cells to rebuild and repair damaged tissues. These aren’t embryonic stem cells but rather adult stem cells, typically derived from bone marrow or adipose (fat) tissue.
How It Works:
- Harvesting Cells: Cells are collected from your own body, usually from the bone marrow in your pelvis or fat tissue in the abdomen or thighs.
- Processing: The cells are processed and sometimes combined with PRP to enhance their effectiveness.
- Injection: The mixture is injected into the painful joint under ultrasound or fluoroscopic guidance.
These cells have the ability to differentiate—meaning they can transform into other types of cells, such as cartilage, bone, or tendon cells. They also release molecules that reduce inflammation and promote healing at the cellular level.
What It’s Used For:
- Moderate to severe osteoarthritis
- Cartilage degeneration
- Chronic joint inflammation
- Joint injuries that haven’t healed with traditional treatments
PRP vs. Cell Therapy: What’s the Difference?
| Feature |
PRP Therapy |
Cell Therapy |
| Source |
Platelets from your blood |
Stem cells from bone marrow or fat |
| Mechanism |
Stimulates healing with growth factors |
Repairs tissue by regenerating new cells |
| Best For |
Mild to moderate joint damage |
Moderate to severe degeneration |
| Invasiveness |
Minimally invasive |
Slightly more invasive (requires tissue harvesting) |
| Cost |
Lower |
Higher |
Think of PRP as a “booster” that speeds up healing, while cell therapy is a “builder” that can regenerate more extensive damage.
What to Expect from Treatment
Procedure:
Both PRP and cell therapy are usually done in an outpatient setting. The procedures typically take 1-2 hours. Since your own cells are used, the risk of allergic reactions is minimal.
Recovery:
- PRP: Mild soreness for a day or two; most people resume normal activity within 24-48 hours.
- Cell Therapy: Slightly longer recovery time due to the harvesting process; some patients may need a few days of rest.
Results:
- Most patients report a gradual reduction in pain over weeks to months.
- Improvements can last anywhere from 6 months to 2 years or more.
- Outcomes vary depending on the severity of the condition, overall health, and adherence to post-treatment guidelines like physical therapy and lifestyle changes.
The Science Behind It
PRP and cell therapy are backed by a growing body of research. For example:
- A 2020 study published in American Journal of Sports Medicine found that PRP injections significantly improved symptoms in patients with knee osteoarthritis over a 12-month period.
- A 2021 meta-analysis concluded that stem cell therapy showed consistent results in improving joint function and reducing pain in osteoarthritis patients, especially when used early in disease progression.
While not a miracle cure, these therapies are helping people delay or even avoid surgery, including joint replacement.
Is It Safe?
Yes—for most patients, PRP and cell therapy are considered safe and well-tolerated. Because the materials come from your own body, the risk of infection or rejection is extremely low. However, like any medical procedure, results aren’t guaranteed, and not everyone is a good candidate.
It’s crucial to consult with a medical provider who specializes in regenerative medicine to determine if these treatments are appropriate for your condition.
Is It Covered by Insurance?
Unfortunately, most insurance companies don’t yet cover PRP or cell therapy, viewing them as experimental. That’s slowly changing as more evidence emerges. Costs can range from a few hundred dollars (for PRP) to several thousand (for cell therapy), so be sure to ask for a cost estimate before committing.
Who’s a Good Candidate?
You might be a good candidate for PRP or cell therapy if you:
- Have chronic joint pain that hasn’t improved with rest, therapy, or medication
- Want to avoid or delay surgery
- Are in good general health
- Are not a smoker (smoking reduces healing)
- Are not severely immunocompromised or on blood thinners
The Future of Joint Pain Treatment
PRP and cell therapy offer a promising new frontier in the treatment of joint pain. These regenerative therapies don’t just cover up symptoms—they tap into the body’s natural ability to heal, rebuild, and regenerate. While they’re not a replacement for all conventional treatments, they can be a powerful tool in the journey to pain relief, better mobility, and improved quality of life.
If joint pain is holding you back, it may be time to consider a regenerative approach. Consult a knowledgeable provider to explore whether PRP or cell therapy is the right path for you.
Disclaimer: This article is for informational purposes only and should not be taken as medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment recommendations.

