Apr 9, 2026
Chronic joint and tendon pain can significantly impact your quality of life—limiting movement, reducing activity levels, and making even everyday tasks uncomfortable. While traditional treatments like medications, physical therapy, and surgery have long been the standard, regenerative medicine is transforming how we approach musculoskeletal injuries. One of the most promising advancements in this space is Platelet-Rich Plasma (PRP) therapy.
PRP therapy offers a minimally invasive, non-surgical option that uses your body’s natural healing mechanisms to repair damaged tissues. But what exactly is PRP, and how does it work? Let’s break it down.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses a concentrated form of your own blood to promote healing. Blood contains several components, including red blood cells, white blood cells, plasma, and platelets. Platelets are especially important because they contain growth factors and proteins that play a key role in tissue repair and regeneration.
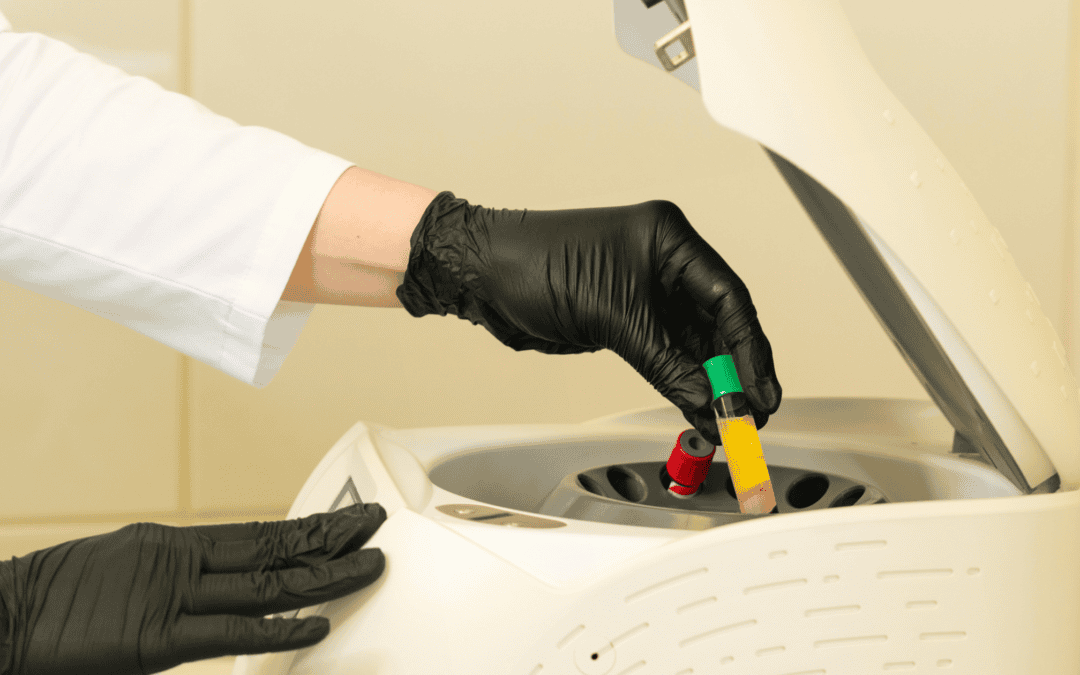
In PRP therapy, a small sample of your blood is drawn and placed in a centrifuge. This process separates the platelets from other blood components, creating a concentrated solution rich in healing factors. The PRP is then injected directly into the injured or painful area.
How PRP Promotes Healing
- Stimulates cell regeneration
- Promotes collagen production
- Improves blood flow to the injured area
- Reduces inflammation
- Accelerates tissue repair
Unlike corticosteroid injections, which primarily reduce inflammation temporarily, PRP targets the underlying cause of pain by supporting actual tissue healing.
Conditions PRP Can Treat
Joint Conditions
- Osteoarthritis (knee, hip, shoulder)
- Degenerative joint disease
- Cartilage injuries
Tendon Injuries
- Tennis elbow (lateral epicondylitis)
- Golfer’s elbow (medial epicondylitis)
- Achilles tendinitis
- Patellar tendinitis (jumper’s knee)
- Rotator cuff injuries
Ligament Injuries
- Partial ligament tears
- Chronic sprains
What to Expect During the Procedure
- Blood Draw: A small amount of blood is taken from your arm.
- Centrifugation: The blood is spun in a centrifuge to isolate the platelet-rich plasma.
- Injection: The PRP is injected into the targeted area, often using ultrasound guidance for precision.
Recovery and Results
One of the major advantages of PRP therapy is its relatively quick recovery time. Because it is a minimally invasive procedure, patients can often return to normal activities within a few days.
However, it’s important to note that PRP is not an instant fix. Since it works by stimulating natural healing, results develop gradually over time. Patients may begin to notice improvement within a few weeks, with continued progress over several months.
Benefits of PRP Therapy
- Minimally invasive
- Uses your body’s own cells
- Targets the root cause of pain
- Reduced downtime
- Versatile treatment option
Are You a Good Candidate for PRP?
PRP therapy is an excellent option for many patients, but it may not be suitable for everyone. Ideal candidates typically include individuals who have chronic joint or tendon pain, have not found relief with conservative treatments, and want to avoid or delay surgery.
PRP vs. Other Treatments
Corticosteroid injections provide short-term relief but do not promote healing. Physical therapy is beneficial but may not be enough for chronic conditions. Surgery can be effective but comes with higher risks and longer recovery times. PRP offers a regenerative alternative without the invasiveness of surgery.
Final Thoughts
If you’re struggling with persistent joint or tendon pain, PRP therapy may offer a safe, effective, and minimally invasive solution. By harnessing your body’s natural healing power, this innovative treatment helps restore function and improve quality of life.
At SDOMG, our team specializes in advanced, patient-centered treatments designed to help you get back to the activities you love. Schedule a consultation today to learn if PRP therapy is right for you.

Mar 26, 2026
Regenerative medicine has become an exciting option for patients seeking relief from chronic pain, joint injuries, and degenerative conditions without surgery. Treatments such as platelet-rich plasma (PRP) injections and other biologic therapies aim to stimulate the body’s natural healing processes rather than simply masking symptoms.
While regenerative treatments can be highly effective, many patients wonder what happens after their procedure. Understanding the recovery process, typical timelines, and how to support healing can help you achieve the best possible results.
The First 24–72 Hours After Treatment
Immediately following a regenerative treatment, it is common to experience mild to moderate soreness at the injection site. This occurs because the treatment intentionally stimulates a healing response within the tissue.
Common short-term symptoms may include:
- Mild swelling or stiffness
- Local tenderness around the injection site
- Temporary increase in pain or discomfort
- Warmth in the treated area
This response is usually a positive sign that the body is beginning its repair process. Most patients find that these symptoms improve within a few days.
Your physician may recommend limiting strenuous activity during this early recovery window to allow the healing process to begin properly.
The First Two Weeks: Early Healing Phase
During the first one to two weeks after treatment, your body is actively working to repair damaged tissues. Many regenerative therapies rely on growth factors and biologic signals that promote cellular repair and tissue regeneration.
During this time, patients may notice:
- Gradual reduction in soreness
- Improved mobility in the treated area
- Subtle improvements in pain levels
Some patients feel improvement fairly quickly, while others may not notice changes until several weeks later. This variation is normal because healing occurs at different rates depending on the individual and the condition being treated.
Weeks 3–6: Tissue Repair and Strengthening
By the third to sixth week following treatment, regenerative therapies are typically well underway. During this stage, tissues continue to remodel and strengthen as the body responds to the biologic signals triggered by the treatment.
Many patients report:
- Reduced inflammation
- Improved joint stability
- Increased range of motion
- Better function during daily activities
This is often when noticeable improvements begin to emerge. However, patients should continue following their provider’s guidance on activity levels and rehabilitation.
Supporting Your Recovery
The success of regenerative treatments is influenced not only by the procedure itself but also by how well patients support their body’s healing process afterward.
Follow Activity Guidelines
Your physician may recommend avoiding heavy exercise, high-impact movements, or strenuous activity for a short period. Gradual reintroduction of movement helps prevent reinjury while tissues are healing.
Participate in Physical Therapy
In some cases, structured physical therapy can enhance recovery. Targeted exercises help strengthen supporting muscles and improve joint stability, which can maximize the benefits of regenerative therapy.
Avoid Anti-Inflammatory Medications
Because regenerative treatments rely on the body’s natural inflammatory healing response, some providers recommend temporarily avoiding medications such as NSAIDs unless directed otherwise.
Maintain Healthy Habits
Proper hydration, balanced nutrition, and quality sleep all support tissue repair and overall healing.
When Will I See Results?
Regenerative medicine works differently than treatments designed for immediate pain relief. Instead of masking symptoms, these therapies aim to address the underlying source of tissue damage.
For this reason, results typically develop gradually.
- 4–6 weeks for early symptom relief
- 8–12 weeks for more significant healing
- 3–6 months for full regenerative effects
The exact timeline depends on the type of treatment, the severity of the condition, and individual health factors.
Follow-Up Care Matters
Follow-up visits allow your physician to monitor healing progress and ensure that recovery is on track. During these appointments, adjustments may be made to activity levels, rehabilitation plans, or additional treatment options if needed.
Some patients may benefit from a series of regenerative treatments, depending on their condition and treatment goals.
A Personalized Healing Journey
Regenerative medicine represents a shift toward treatments that work with the body’s natural biology rather than relying solely on medications or surgery. While results take time to develop, many patients appreciate the potential for long-term improvement and restored function.
If you are considering regenerative treatments or have recently undergone a procedure, staying informed and actively participating in your recovery plan can make a meaningful difference in your outcome.
Working closely with your care team helps ensure that your healing journey is safe, effective, and aligned with your long-term health goals.

Jan 23, 2026
Platelet-rich plasma (PRP) injections have gained attention as a regenerative treatment option for patients seeking relief from joint, tendon, ligament, and soft tissue pain. Often used in orthopedics, sports medicine, and pain management, PRP offers a minimally invasive approach designed to support the body’s natural healing processes. If you’re considering PRP therapy, understanding how it works, what it treats, and what to expect can help you make an informed decision.
What Are PRP Injections?
PRP stands for platelet-rich plasma. Platelets are a natural component of blood best known for their role in clotting, but they also contain growth factors that support tissue repair.
During a PRP procedure:
- A small amount of the patient’s blood is drawn
- The blood is spun in a centrifuge to concentrate the platelets
- The platelet-rich portion is injected into the targeted area
Because PRP is derived from the patient’s own blood, the risk of allergic reaction or rejection is extremely low.
How PRP Supports Healing
PRP works by delivering a high concentration of growth factors directly to injured or degenerative tissue. These growth factors may:
- Promote tissue repair
- Reduce inflammation
- Support collagen production
- Encourage cellular regeneration
Rather than simply masking pain, PRP aims to improve the underlying tissue environment to support longer-term healing.
Conditions Commonly Treated with PRP
PRP injections may be recommended for a variety of musculoskeletal conditions, including:
- Knee, hip, and shoulder osteoarthritis
- Tendon injuries (such as tennis elbow or Achilles tendinopathy)
- Ligament sprains
- Chronic joint pain
- Muscle injuries
- Certain spine-related soft tissue conditions
PRP is often considered when conservative treatments like physical therapy or medications have not provided sufficient relief.
What to Expect During and After Treatment
PRP injections are typically performed in an outpatient setting and usually take less than an hour.
After the procedure:
- Mild soreness or swelling at the injection site is common
- Patients are often advised to limit strenuous activity for several days
- Pain relief and functional improvement may develop gradually over weeks
Because PRP stimulates a biological healing response, results are not immediate. Some patients may require a series of injections depending on the condition being treated.
Is PRP Right for Everyone?
While PRP is generally safe, it may not be appropriate for all patients. Factors such as:
- Severity of tissue damage
- Overall health
- Blood disorders or active infections
- Treatment goals
should be discussed with a qualified medical provider. PRP is not a replacement for surgery in severe structural damage, but it may help delay or reduce the need for more invasive procedures.
It’s also important to note that PRP is considered a biologic therapy, and coverage varies because it is not universally approved by U.S. Food and Drug Administration for all indications.
PRP vs. Steroid Injections
Unlike corticosteroid injections, which primarily reduce inflammation and pain temporarily, PRP aims to support tissue repair. Steroids may provide faster relief but can weaken tissues with repeated use. PRP may take longer to show results but is often chosen for its regenerative potential.
Final Thoughts
PRP injections represent an evolving approach in regenerative and pain medicine, offering patients a minimally invasive option that works with the body’s natural healing abilities. While results vary, many patients find PRP to be a valuable part of a comprehensive, non-surgical treatment plan.
If you’re experiencing ongoing joint or soft tissue pain, a consultation with a pain management or regenerative medicine specialist can help determine whether PRP is an appropriate option for you.

Jan 9, 2026
For many people living with chronic joint, tendon, or spine pain, surgery can feel like an inevitable next step. While surgery is sometimes necessary, it is not always the only option. Advances in regenerative medicine have created new possibilities for pain relief and tissue healing that may help some patients delay, or even avoid, surgical intervention.
Understanding how regenerative treatments work, who may benefit, and their limitations can help patients make informed decisions about their care.
What Are Regenerative Treatments?
Regenerative treatments are therapies designed to support the body’s natural healing processes rather than simply masking pain or removing damaged tissue. Instead of cutting or replacing structures, these treatments aim to encourage repair at the cellular level.
Common regenerative approaches include platelet-based therapies and other biologic injections that are derived from the patient’s own body. These treatments are most often used for musculoskeletal conditions affecting joints, ligaments, tendons, and certain spinal structures.
How Regenerative Treatments May Reduce the Need for Surgery
Surgery is typically recommended when pain and functional limitations persist despite conservative care. Regenerative therapies may help fill the gap between traditional treatments and surgical intervention by addressing underlying tissue damage earlier in the disease process.
Potential ways regenerative treatments may help avoid surgery include:
• Reducing inflammation that contributes to pain and stiffness
• Supporting tissue repair in tendons, ligaments, and cartilage
• Improving joint function and mobility
• Slowing degenerative changes when used appropriately
• Enhancing recovery when combined with physical therapy
For patients with mild to moderate degeneration or soft tissue injuries, these effects may significantly improve quality of life without the risks and recovery time associated with surgery.
Conditions Where Regenerative Treatments May Be Helpful
Regenerative therapies are not a cure-all, but they may be beneficial for certain conditions, including:
• Osteoarthritis of the knee, shoulder, or hip
• Tendon injuries such as tennis elbow or rotator cuff tendinopathy
• Ligament sprains or chronic instability
• Mild to moderate degenerative disc-related pain
• Joint overuse injuries
Patients with advanced joint collapse, severe structural damage, or progressive neurological symptoms may still require surgical evaluation.
Benefits Compared to Surgery
One of the primary reasons patients explore regenerative treatments is the desire to avoid surgery-related risks and downtime.
Potential advantages include:
• Minimally invasive procedures
• Shorter recovery periods
• Reduced risk of complications
• Outpatient treatment setting
• Use of the patient’s own biological materials
These factors make regenerative therapies an appealing option for patients who want to remain active or who may not be ideal surgical candidates.
Limitations and Realistic Expectations
While regenerative treatments can be effective for some patients, they are not guaranteed to eliminate pain or fully reverse degeneration. Results can vary based on the condition being treated, the severity of damage, overall health, and adherence to a rehabilitation plan.
It is also important to understand that regenerative treatments work best as part of a comprehensive pain management strategy that may include physical therapy, activity modification, and lifestyle changes.
Who Is a Good Candidate?
Good candidates for regenerative treatments often include patients who:
• Have not found sufficient relief with medications or therapy
• Want to delay or avoid surgery
• Have mild to moderate tissue damage
• Are willing to commit to follow-up care and rehabilitation
A thorough evaluation by a pain management or spine specialist is essential to determine whether regenerative treatments are appropriate.
The Importance of Personalized Care
No two patients are the same, and treatment decisions should never be one-size-fits-all. A personalized approach allows providers to weigh the potential benefits of regenerative therapies against other conservative or interventional options.
In some cases, regenerative treatments may delay surgery for years. In others, they may reduce pain enough to make daily activities manageable without surgery.
Final Thoughts
Regenerative treatments represent an exciting and evolving area of pain management. While they may not replace surgery for everyone, they offer a promising option for patients seeking less invasive solutions for chronic pain and musculoskeletal conditions.
If you are considering regenerative treatments, discussing your goals, expectations, and long-term plan with a qualified pain specialist can help you determine whether this approach may help you avoid, or at least postpone, surgery.
Dec 24, 2025
Tendon injuries and chronic tendon degeneration — often called tendinopathy — are common yet stubbornly difficult to treat. From athletes pushing through pain to older adults coping with age-related wear, tendon issues can severely limit movement and quality of life. Traditional approaches like rest, physical therapy, anti-inflammatory medications, or surgery remain standard, but many people still struggle with lingering pain and functional limitations. Thankfully, emerging regenerative medicine approaches offer new hope — and a fundamentally different way of thinking about healing.
What Makes Tendons Hard to Heal?
Unlike other tissues, tendons have a poor blood supply, limiting their natural healing ability. When injured, tendons often form scar tissue rather than regenerating healthy tendon fibers, which can lead to chronic pain and repeated injury cycles. Aging, repetitive strain, and certain systemic conditions can worsen this process, making degeneration a long-lasting problem.
Regenerative Medicine: Healing Over Scarring
Regenerative medicine offers therapies that go beyond simply reducing symptoms. Instead, these treatments aim to stimulate the body’s own healing mechanisms, potentially leading to more complete tissue repair.
Here are some of the most studied and promising options:
1. Platelet-Rich Plasma (PRP) Therapy
PRP involves drawing a patient’s own blood, concentrating the platelets, and then injecting this platelet-rich plasma into the injured tendon. Platelets release growth factors that may help stimulate tendon cell activity, reduce inflammation, and support repair. PRP is one of the most widely used regenerative treatments for tendon injuries and is often offered as an outpatient procedure with minimal downtime.
2. Stem Cell-Based Therapies
Mesenchymal stem cells (from bone marrow or adipose tissue) are being researched for their ability to differentiate into tendon-like cells and secrete healing signals. Early studies suggest they could help modulate inflammation and support regeneration. Although clinical evidence continues to evolve and large, high-quality trials are still needed, many researchers view stem cells as a key frontier in tendon repair science.
3. Next-Generation Blood Factor Treatments
Beyond traditional PRP, newer approaches aim to isolate specific growth factors or concentrate regenerative signals more precisely. Plasma-Derived Factor treatments (like PDF-FD) extract and concentrate key proteins from blood, then deliver them directly to the injured site — potentially enhancing healing responses.
Other Frontiers: Biomaterials & Tissue Engineering
Researchers are also looking at biomaterials, scaffolds, and guided tissue engineering as ways to support tendon regeneration structurally and biologically. These approaches use engineered materials to provide a framework for tendon cells to grow — which, in theory, could rebuild tissue more like the original tendon. Although many of these are still in early stages, they represent exciting future directions.
What to Know Before Considering Regenerative Treatments
- Evidence varies: While some regimens are backed by clinical research, others are still experimental. The strength of evidence for effectiveness differs across therapies, and not all treatments are universally accepted by mainstream medical societies.
- Regulation and safety: Some regenerative therapies are regulated, others are offered at clinics without standardized oversight. Discuss risks, benefits, and alternatives with a qualified provider.
- Not a magic bullet: Regenerative treatments are most effective when combined with physical therapy, lifestyle changes, and proper loading programs to support tendon health.
Conclusion
Tendon injuries and degeneration don’t have to be resigned to “rest and wait.” The emerging world of regenerative medicine showcases promising paths to enhance healing, stimulate regeneration, and restore function — even for chronic tendon issues. As research advances and clinical evidence grows, these biologic solutions may reshape how we approach tendon care in the years ahead.

Dec 5, 2025
As temperatures drop, many people notice their joints becoming stiff, achy, or more painful than usual. Winter weather can aggravate conditions like arthritis, tendon injuries, and chronic joint degeneration—making it harder to stay active and comfortable. While traditional treatments such as NSAIDs, bracing, and heat therapy offer temporary relief, patients looking for longer-term improvement often turn to regenerative medicine.
Here’s why winter is actually one of the best times to explore regenerative options like PRP (platelet-rich plasma), orthobiologics, and cell-based therapies.
Why Joints Hurt More in Winter
Many patients describe their joints as “weather predictors,” especially when cold air arrives. Several factors explain why winter intensifies joint discomfort:
1. Changes in Barometric Pressure
Dropping pressure can cause joint tissues to expand slightly, leading to increased stiffness or pain—especially in joints already affected by inflammation or degeneration.
2. Cold Muscles = Stiffer, Tighter Movement
Cold temperatures reduce muscle elasticity. This places extra strain on tendons, ligaments, and joints.
3. Reduced Activity Levels
Shorter days and cold weather reduce physical activity, which weakens supportive muscles and worsens joint mobility.
4. Increased Inflammation
For some individuals, cold stress increases inflammatory responses, intensifying pain in arthritic or injured joints.
Why Winter Is a Smart Time to Choose Regenerative Medicine
Regenerative therapies work by supporting the body’s natural ability to repair and restore damaged tissues. During the winter, this approach can be particularly beneficial for several reasons.
1. Winter Often Marks a Natural Slowdown—Perfect for Recovery
Many people slow their routines during the colder months. This makes it easier to schedule the brief downtime required after regenerative injections.
2. Reduced Activity Helps Regeneration Work Better
After treatments like PRP, patients need a window of lower impact activity. Winter’s pace naturally aligns with this healing phase.
3. Get Ahead of Spring Activity
Whether you’re preparing for gardening, sports, travel, or outdoor activities, winter treatment gives your joints time to heal so you can be more active (and pain-free) when spring arrives.
4. Regenerative Medicine Addresses the Root Cause
Unlike medications that only mask pain, regenerative therapies aim to:
- reduce inflammation
- improve blood flow
- support tissue repair
- slow or reverse degenerative processes
This makes it an ideal option for chronic winter flares.
5. Less Reliance on Seasonal Pain Medications
Patients often notice increased medication use during colder months. Regenerative care can help reduce dependence on pills or repetitive steroid injections.
Common Joint Issues Treated with Regenerative Therapy in Winter
Winter pain tends to flare in:
- knees (arthritis, meniscus issues, cartilage loss)
- hips (labral tears, early arthritis)
- shoulders (rotator cuff injuries, tendonitis)
- elbows (tendon degeneration)
- ankles and feet (Achilles issues, plantar fasciitis)
- spine joints (facet arthritis)
Regenerative medicine helps stabilize and strengthen these areas while reducing pain.
Types of Regenerative Treatments That Work Well in Winter
PRP Injections (Platelet-Rich Plasma)
Uses your own platelets to decrease inflammation and stimulate tissue repair.
Orthobiologics
Includes growth-factor-rich injections, micro-fat grafting, and other biologic agents that support healing.
Cell-Based Therapies
Derived from bone marrow or fat tissue to promote repair in more advanced degeneration.
Your provider will recommend options based on imaging, severity, and your activity goals.
Supporting Joint Care Through the Cold Season
Regenerative medicine works best when paired with targeted lifestyle strategies. Consider adding:
- winter-appropriate movement (indoor walking, stretching, low-impact exercise)
- anti-inflammatory nutrition
- joint-warming routines (heat therapy, warm showers before activity)
- physical therapy for mobility and strength
- proper winter footwear and traction
These habits help maintain the benefits of regenerative treatment and keep winter symptoms under control.
Is Regenerative Medicine Right for You This Winter?
If cold weather consistently makes your joint pain worse—or if you’re tired of managing symptoms year after year—this may be the perfect time to explore regenerative options. These treatments are especially helpful if:
- conservative therapies have stopped working
- pain interferes with winter activity
- you want a longer-term, non-surgical approach
- you prefer natural healing over medications
- you want to prepare your body for an active spring
Winter doesn’t have to be painful. With the right regenerative plan, you can stay mobile, reduce inflammation, and give your joints the healing support they need.





