Apr 9, 2026
Chronic joint and tendon pain can significantly impact your quality of life—limiting movement, reducing activity levels, and making even everyday tasks uncomfortable. While traditional treatments like medications, physical therapy, and surgery have long been the standard, regenerative medicine is transforming how we approach musculoskeletal injuries. One of the most promising advancements in this space is Platelet-Rich Plasma (PRP) therapy.
PRP therapy offers a minimally invasive, non-surgical option that uses your body’s natural healing mechanisms to repair damaged tissues. But what exactly is PRP, and how does it work? Let’s break it down.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses a concentrated form of your own blood to promote healing. Blood contains several components, including red blood cells, white blood cells, plasma, and platelets. Platelets are especially important because they contain growth factors and proteins that play a key role in tissue repair and regeneration.
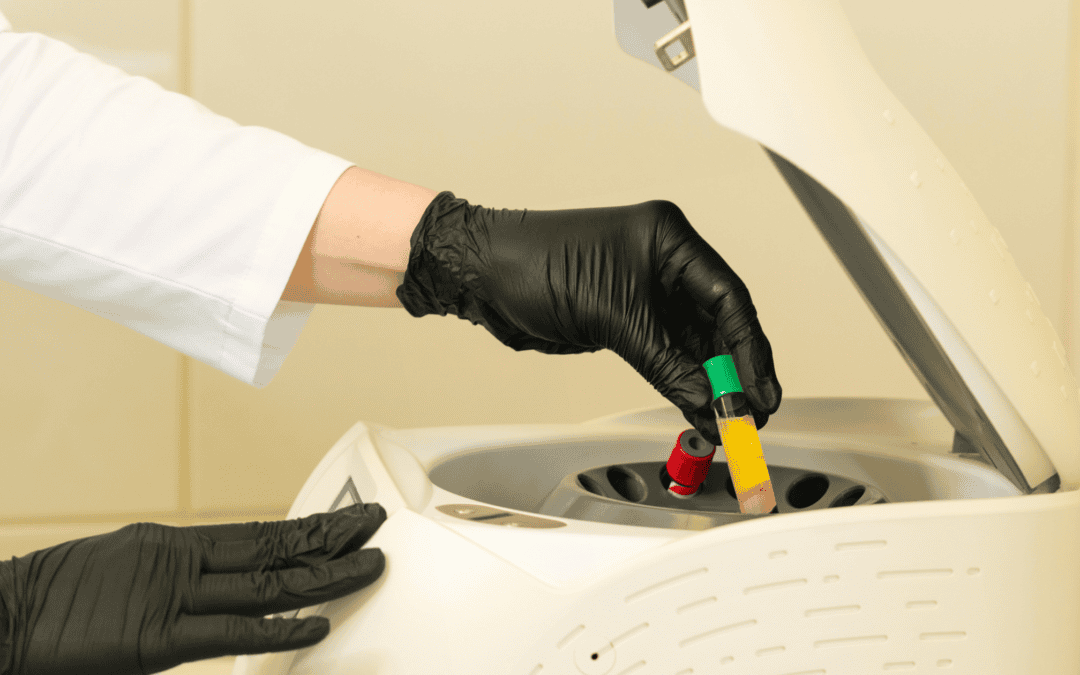
In PRP therapy, a small sample of your blood is drawn and placed in a centrifuge. This process separates the platelets from other blood components, creating a concentrated solution rich in healing factors. The PRP is then injected directly into the injured or painful area.
How PRP Promotes Healing
- Stimulates cell regeneration
- Promotes collagen production
- Improves blood flow to the injured area
- Reduces inflammation
- Accelerates tissue repair
Unlike corticosteroid injections, which primarily reduce inflammation temporarily, PRP targets the underlying cause of pain by supporting actual tissue healing.
Conditions PRP Can Treat
Joint Conditions
- Osteoarthritis (knee, hip, shoulder)
- Degenerative joint disease
- Cartilage injuries
Tendon Injuries
- Tennis elbow (lateral epicondylitis)
- Golfer’s elbow (medial epicondylitis)
- Achilles tendinitis
- Patellar tendinitis (jumper’s knee)
- Rotator cuff injuries
Ligament Injuries
- Partial ligament tears
- Chronic sprains
What to Expect During the Procedure
- Blood Draw: A small amount of blood is taken from your arm.
- Centrifugation: The blood is spun in a centrifuge to isolate the platelet-rich plasma.
- Injection: The PRP is injected into the targeted area, often using ultrasound guidance for precision.
Recovery and Results
One of the major advantages of PRP therapy is its relatively quick recovery time. Because it is a minimally invasive procedure, patients can often return to normal activities within a few days.
However, it’s important to note that PRP is not an instant fix. Since it works by stimulating natural healing, results develop gradually over time. Patients may begin to notice improvement within a few weeks, with continued progress over several months.
Benefits of PRP Therapy
- Minimally invasive
- Uses your body’s own cells
- Targets the root cause of pain
- Reduced downtime
- Versatile treatment option
Are You a Good Candidate for PRP?
PRP therapy is an excellent option for many patients, but it may not be suitable for everyone. Ideal candidates typically include individuals who have chronic joint or tendon pain, have not found relief with conservative treatments, and want to avoid or delay surgery.
PRP vs. Other Treatments
Corticosteroid injections provide short-term relief but do not promote healing. Physical therapy is beneficial but may not be enough for chronic conditions. Surgery can be effective but comes with higher risks and longer recovery times. PRP offers a regenerative alternative without the invasiveness of surgery.
Final Thoughts
If you’re struggling with persistent joint or tendon pain, PRP therapy may offer a safe, effective, and minimally invasive solution. By harnessing your body’s natural healing power, this innovative treatment helps restore function and improve quality of life.
At SDOMG, our team specializes in advanced, patient-centered treatments designed to help you get back to the activities you love. Schedule a consultation today to learn if PRP therapy is right for you.

Feb 20, 2026
Chronic joint, tendon, and ligament pain can make everyday activities feel like a challenge. When conservative treatments like rest, physical therapy, and anti-inflammatory medications are not enough, injection therapies are often the next step. Two of the most common options are Platelet-Rich Plasma (PRP) therapy and cortisone (steroid) injections.
While both treatments are used to relieve pain and inflammation, they work in very different ways. Understanding the differences can help you make an informed decision about your care.
What Is PRP Therapy?
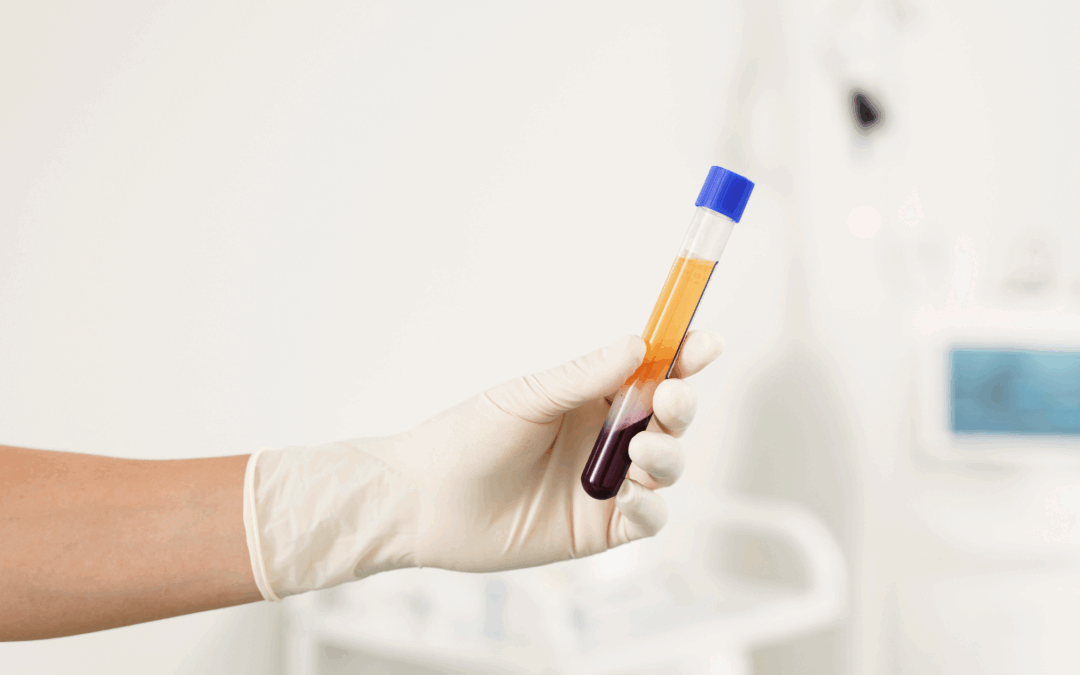
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses your body’s own healing properties. A small sample of your blood is drawn and placed in a centrifuge to separate and concentrate the platelets. These platelets contain growth factors that help support tissue repair.
The concentrated PRP is then injected into the injured or painful area, such as:
- Knee osteoarthritis
- Tendon injuries (like tennis elbow or Achilles tendonitis)
- Shoulder pain
- Hip pain
- Mild ligament injuries
PRP focuses on promoting healing at the source of the problem rather than simply masking symptoms.
What Are Cortisone Injections?
Cortisone injections contain a powerful anti-inflammatory medication (a corticosteroid). When injected into a joint or soft tissue, cortisone quickly reduces inflammation and swelling, often providing rapid pain relief.
Cortisone injections are commonly used for:
- Arthritis flare-ups
- Bursitis
- Tendinitis
- Acute joint inflammation
- Spinal joint irritation
They are especially helpful when inflammation is severe and immediate symptom relief is needed.
How They Work: Regeneration vs. Suppression
The biggest difference between PRP and cortisone lies in how they treat pain.
PRP:
- Stimulates tissue healing
- Encourages cellular repair
- May improve tissue quality over time
- Often used for chronic or degenerative conditions
Cortisone:
- Reduces inflammation quickly
- Suppresses the immune response
- Primarily addresses symptoms
- Often used for acute inflammation or flare-ups
PRP aims to repair. Cortisone aims to calm inflammation.
Speed of Relief
Cortisone injections often provide relief within a few days. This makes them appealing for patients who need fast improvement, such as before an event or during a severe flare-up.
PRP therapy typically takes longer to show results. Some patients notice improvement within a few weeks, but full benefits may take several weeks to months as the tissue heals.
Duration of Results
Cortisone relief may last weeks to several months, but repeated injections can potentially weaken tissues over time.
PRP results may take longer to appear but can last longer because the treatment supports healing rather than temporary suppression.
Safety and Side Effects
Both treatments are generally safe when performed by experienced providers.
Cortisone risks may include:
- Temporary pain flare after injection
- Tissue weakening with repeated use
- Elevated blood sugar (important for diabetic patients)
PRP risks may include:
- Temporary soreness at the injection site
- Mild swelling
- Minimal risk of allergic reaction since it uses your own blood
Because PRP uses your body’s natural components, it carries a low risk of adverse reactions.
Which Treatment Is Right for You?
The right choice depends on several factors:
- Severity of pain and inflammation
- Treatment goals (short-term relief vs. long-term healing)
- Other health issues
- Previous treatment history
In some cases, cortisone may be appropriate to quickly calm severe inflammation before beginning a longer-term strategy like PRP and rehabilitation.
Personalized Care at SDOMG
At SDOMG, treatment decisions are based on your specific diagnosis, activity level, and long-term goals. Whether you need fast relief from a painful flare-up or a regenerative approach to support tissue healing, we help guide you toward the option that best supports your recovery.
If you are experiencing persistent joint or tendon pain, schedule a consultation to discuss whether PRP therapy, cortisone injections, or another treatment approach is right for you.
Your recovery plan should be as individualized as you are.
May 30, 2025
In the high-stakes world of sports, injury recovery time can define the trajectory of an athlete’s career. Whether it’s a torn ligament, chronic tendonitis, or a nagging joint issue, athletes are always seeking faster and more effective ways to heal and return to peak performance. This is where regenerative medicine, particularly Platelet-Rich Plasma (PRP) and Bone Marrow Aspirate Concentrate (BMAC), has emerged as a transformative solution.
These innovative therapies leverage the body’s own biological resources to accelerate tissue repair, reduce inflammation, and minimize downtime. In this post, we’ll delve into how PRP and BMAC are being used to help athletes recover faster from injuries and why they’re gaining popularity in sports medicine.
What is Regenerative Medicine?
Regenerative medicine refers to treatments that aim to restore normal function by repairing or regenerating damaged tissues or organs using the body’s own healing mechanisms. Unlike traditional treatments that manage symptoms or rely on surgical intervention, regenerative therapies work at the cellular level to enhance the natural healing process.
Among the most widely accepted and commonly used forms of regenerative medicine in athletic recovery are Platelet-Rich Plasma (PRP) and Bone Marrow Aspirate Concentrate (BMAC).
Platelet-Rich Plasma (PRP): Supercharging the Body’s Healing Process
PRP therapy involves concentrating platelets from a patient’s own blood and injecting them into the injured area. Platelets are rich in growth factors—biological signals that stimulate tissue repair and regeneration.
How PRP Works
- Blood Collection: A small amount of the athlete’s blood is drawn, typically from the arm.
- Centrifugation: The blood is spun in a centrifuge to separate platelets from other components.
- Injection: The resulting PRP—plasma with a high concentration of platelets—is injected directly into the injured tissue under ultrasound guidance.
PRP Applications in Sports Injuries
PRP is used extensively for musculoskeletal injuries common in sports, including:
- Tendonitis (e.g., tennis elbow, Achilles tendonitis)
- Ligament sprains (e.g., MCL sprains)
- Muscle tears
- Joint degeneration (e.g., mild osteoarthritis)
Benefits of PRP for Athletes
- Accelerated Healing: PRP delivers concentrated growth factors to the injury site, promoting faster tissue regeneration.
- Reduced Inflammation: The therapy helps modulate the inflammatory response, which can reduce pain and swelling.
- Minimally Invasive: As an injection-based treatment, PRP avoids the trauma of surgery and its associated risks.
- Shorter Downtime: Many athletes return to training and competition sooner than with traditional rehabilitation alone.
Bone Marrow Aspirate Concentrate (BMAC): A Rich Source of Healing Cells
Bone Marrow Aspirate Concentrate (BMAC) is another autologous (self-derived) regenerative therapy. It involves aspirating bone marrow—typically from the iliac crest (hip bone)—and concentrating the healing components for injection into injured tissues.
What’s in BMAC?
BMAC is rich in:
- Platelets: Similar to PRP, these deliver growth factors that aid in healing.
- White blood cells: Important for modulating inflammation and fighting infection.
- Progenitor cells: These assist in the repair and regeneration of damaged tissue, especially in bone and cartilage injuries.
How BMAC Works
- Harvesting: Bone marrow is collected using a minimally invasive aspiration procedure.
- Processing: The marrow is processed to concentrate the regenerative components.
- Injection: The final concentrate is injected into the site of injury.
BMAC Applications in Athletic Recovery
BMAC is especially useful in treating:
- Cartilage injuries
- Joint degeneration
- Non-healing bone fractures
- Chronic tendon and ligament injuries
Benefits of BMAC for Athletes
- Deep Tissue Repair: BMAC is effective for more complex or severe injuries, especially those involving cartilage and bone.
- One-Time Treatment: In many cases, a single BMAC injection can provide significant improvement.
- Natural and Autologous: As with PRP, BMAC uses the athlete’s own biological material, minimizing risk of rejection or complications.
- Enhanced Recovery: Athletes often experience reduced pain, improved function, and quicker return to play.
Clinical Evidence
BMAC has been studied for its potential in treating cartilage defects and bone injuries. A 2016 clinical trial published in Orthopaedic Journal of Sports Medicine showed that athletes with knee cartilage lesions treated with BMAC experienced meaningful improvements in function and pain relief.
PRP vs. BMAC: Which is Better for Athletic Injuries?
While both PRP and BMAC are powerful tools in regenerative medicine, they serve different roles depending on the nature and severity of the injury.
| Aspect |
PRP |
BMAC |
| Source |
Blood |
Bone marrow |
| Best For |
Soft tissue injuries, mild arthritis |
Bone/cartilage injuries, chronic damage |
| Processing Complexity |
Low |
Moderate to high |
| Healing Potential |
Moderate |
Higher (especially for deeper injuries) |
| Invasiveness |
Minimally invasive (blood draw) |
Slightly more invasive (bone aspiration) |
In many sports medicine clinics, practitioners assess the injury type, severity, and the athlete’s goals to determine which therapy—or combination—is most suitable.
The Athlete’s Perspective: Real-World Impact
Athletes from every discipline, from weekend warriors to Olympic gold medalists, are increasingly turning to PRP and BMAC to speed up recovery. High-profile sports figures like Tiger Woods, Rafael Nadal, and Kobe Bryant have reportedly used PRP therapy to overcome injuries and return to elite competition.
For athletes, the primary appeal of these treatments lies in the combination of effectiveness and reduced recovery time. In a world where every game, match, or race matters, shaving weeks off a recovery timeline can make a critical difference.
Limitations and Considerations
While PRP and BMAC are promising, they’re not miracle cures. Effectiveness can vary based on:
- Type and chronicity of injury
- Overall health and age of the athlete
- Technique and quality of the preparation
Additionally, these treatments may not be covered by insurance and can be costly, though many athletes see them as worthwhile investments in their careers and long-term joint health.
Conclusion
Regenerative medicine is reshaping the future of sports injury recovery. PRP and BMAC stand at the forefront, offering biologically-based, minimally invasive options to accelerate healing and reduce downtime for athletes of all levels. As research continues and technology advances, the integration of these therapies into mainstream sports medicine is expected to grow—giving injured athletes a faster, safer path back to the game.
Whether you’re a professional athlete or an active individual looking to get back on your feet, PRP and BMAC offer compelling alternatives to surgery and long-term medications. Always consult with a qualified sports medicine specialist to determine the best course of action tailored to your specific condition and goals.
May 23, 2025
When dealing with chronic joint pain, tendon injuries, or arthritis, many patients are presented with two popular options for relief: PRP (Platelet-Rich Plasma) therapy and cortisone (corticosteroid) injections. Both treatments are administered via injection and have shown efficacy in reducing inflammation and pain. However, they work through vastly different mechanisms, and their long-term outcomes vary significantly.
So, which one is better for long-term healing?
In this blog post, we’ll explore the key differences between PRP and cortisone injections, examine their benefits and limitations, and help you make a more informed decision based on your condition and goals.
Understanding the Basics
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses a patient’s own blood to promote healing. Here’s how it works:
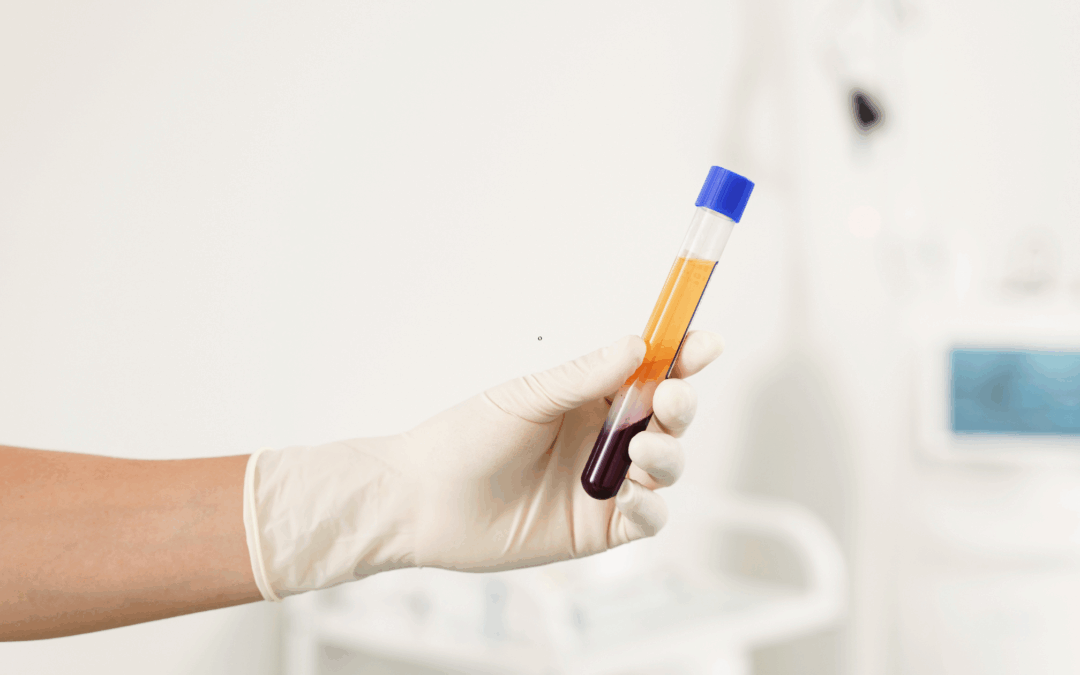
- A small amount of the patient’s blood is drawn.
- It is spun in a centrifuge to concentrate the platelets and growth factors.
- This concentrated plasma is injected into the injured area.
PRP is rich in proteins and growth factors that support tissue regeneration, reduce inflammation, and accelerate healing. It is most commonly used for:
- Tendon injuries (like tennis elbow or Achilles tendinopathy)
- Ligament sprains
- Osteoarthritis
- Muscle tears
- Post-surgical recovery
What Are Cortisone Injections?
Cortisone injections are a form of corticosteroid medication used to reduce inflammation and suppress immune system activity. They don’t promote healing but instead provide symptomatic relief by decreasing swelling and irritation.
Common uses include:
- Arthritis (especially in knees, hips, and shoulders)
- Bursitis
- Tendinitis
- Back pain or nerve inflammation (like sciatica)
Mechanism of Action: Relief vs. Regeneration
This is the key point of differentiation between PRP and cortisone.
- Cortisone works like a fire extinguisher: it quickly reduces inflammation and pain. However, this effect is temporary, and repeated use can actually degrade tissue over time, especially tendons and cartilage.
- PRP, in contrast, aims to heal the underlying problem. By stimulating the body’s natural healing processes, PRP supports long-term recovery rather than just short-term pain relief.
Efficacy: What Does the Research Say?
Short-Term Relief
Cortisone generally outperforms PRP in the short term. Within days of the injection, patients often report significant pain relief. This makes cortisone a go-to treatment for acute flare-ups or when quick pain reduction is critical.
PRP, on the other hand, has a delayed onset of action. It can take a few weeks to start seeing improvement, with the best results often appearing several months after treatment.
Long-Term Results
Multiple studies suggest that PRP may provide superior long-term outcomes for certain musculoskeletal conditions:
- A 2020 meta-analysis published in The American Journal of Sports Medicine showed that PRP injections yielded better long-term relief for knee osteoarthritis compared to corticosteroids.
- In cases of tendinopathy, like tennis elbow or patellar tendinitis, PRP has demonstrated more sustainable improvements in pain and function over 6-12 months.
- A 2015 study in the Journal of Orthopaedic Surgery and Research found that PRP significantly improved pain and mobility in chronic plantar fasciitis patients, while cortisone offered only short-term relief with diminishing benefits.
Risks and Side Effects
Cortisone Injections:
While cortisone is generally safe for occasional use, repeated injections can have side effects, including:
- Tissue degeneration (especially in tendons and cartilage)
- Joint infection (rare but serious)
- Elevated blood sugar (in diabetic patients)
- Skin discoloration or thinning
Repeated cortisone use has been linked with weakened tendons, potentially leading to ruptures. Because of this, doctors often limit cortisone injections to 3-4 times per year per site.
PRP Injections:
Since PRP uses the patient’s own blood, allergic reactions are virtually nonexistent. Side effects are typically mild:
- Temporary soreness or swelling at the injection site
- Bruising
- Mild inflammation (as healing response begins)
Because it doesn’t introduce synthetic substances, PRP is considered low-risk, even with multiple treatments.
Cost and Accessibility
One of the biggest barriers to PRP therapy is cost.
- Cortisone injections are widely covered by insurance and are relatively inexpensive.
- PRP injections, on the other hand, are not usually covered by insurance and can cost $500 to $2,000 per session, depending on location and complexity.
However, when factoring in the potential need for repeated cortisone injections and long-term degeneration risks, PRP might be more cost-effective over time—particularly if it helps you avoid surgery or further interventions.
Recovery Time
- Cortisone typically requires little to no downtime, and patients often resume normal activity quickly.
- PRP may involve short-term rest and modified activity for a few days to a week as the healing process begins. Some patients benefit from physical therapy in conjunction with PRP to optimize outcomes.
Who Should Consider PRP?
PRP is especially promising for:
- Athletes who want to recover without relying on long-term steroid use
- Middle-aged adults with early osteoarthritis hoping to avoid joint replacement
- Active individuals with tendon injuries or ligament sprains
- Patients who’ve had limited relief from cortisone injections or other conservative treatments
Because it promotes actual healing rather than masking symptoms, PRP can be a game-changer for long-term joint and soft tissue health.
When Is Cortisone the Better Option?
Cortisone may be a better choice if you:
- Need quick pain relief for a flare-up
- Have acute inflammation that needs to be controlled
- Are not a candidate for PRP due to cost or blood disorders
- Have a short timeline (e.g., trying to manage symptoms before an important event or surgery)
It’s also worth noting that cortisone can sometimes be used in conjunction with other treatments (like physical therapy or bracing) as part of a larger strategy.
Combination Therapy: Can You Use Both?
Some clinicians explore combined approaches, where cortisone is used initially for pain relief, followed by PRP to promote healing. While more research is needed in this area, early anecdotal reports suggest that staggered treatments may offer the best of both worlds in certain cases.
However, injecting cortisone before PRP may reduce the effectiveness of PRP due to steroid-induced suppression of the body’s healing response. Therefore, timing and sequence matter, and this approach should only be considered under the guidance of an experienced physician.
Final Verdict: PRP vs. Cortisone for Long-Term Healing
So, which is better for long-term healing?
- If you’re looking for fast pain relief and temporary control of inflammation: Cortisone is your best bet.
- If you’re aiming for lasting improvement and true healing of damaged tissue: PRP is likely the better choice.
While cortisone has its place in managing inflammation, PRP aligns more closely with regenerative medicine goals—not just suppressing symptoms, but addressing the root cause.
That said, every patient is different. Factors like age, injury severity, medical history, and financial resources should all play into your decision. Always consult with a knowledgeable sports medicine or orthopedic specialist to determine the best approach for your unique situation.
Conclusion
As medical science advances, patients now have more options than ever to manage pain and support healing. PRP therapy represents a shift toward regenerative treatment strategies, while cortisone remains a reliable tool for managing acute symptoms.
In the end, choosing between PRP and cortisone isn’t just about “which is better”—it’s about choosing the right tool for the job, with an eye toward both short-term comfort and long-term recovery.
If you’re dealing with a chronic injury or joint issue and want to explore your options, talk to a healthcare provider familiar with both approaches. With the right guidance, you can chart a path to recovery that fits your goals, your lifestyle, and your body’s unique needs.

Apr 23, 2025
Arthritis affects over 58 million adults in the United States alone, making it a leading cause of disability and pain. Traditionally, treatment options have focused on symptom management through medications, physical therapy, and, in severe cases, joint replacement surgery. However, recent advances in regenerative medicine are changing the landscape of arthritis care by offering promising, non-surgical alternatives that aim to repair and restore damaged tissues.
In this post, we’ll explore the latest regenerative medicine techniques used to treat arthritis, how they work, and why they’re generating excitement among physicians and patients alike.
Understanding Arthritis and Its Impact
Arthritis is not a single disease but a term that covers more than 100 different types of joint conditions. The most common forms are osteoarthritis (OA) and rheumatoid arthritis (RA):
- Osteoarthritis is a degenerative joint disease where the cartilage that cushions bones wears down over time.
- Rheumatoid arthritis is an autoimmune condition where the immune system attacks the synovial lining of the joints, causing inflammation and tissue damage.
Regardless of the type, arthritis often leads to joint pain, stiffness, decreased mobility, and a diminished quality of life.
Why Patients Seek Non-Surgical Options
Joint replacement surgery, while effective, comes with risks: infection, blood clots, lengthy recovery periods, and even the potential for implant failure over time. Many patients are not ready—or suitable candidates—for surgery and seek less invasive options to manage symptoms and improve joint function.
That’s where regenerative medicine steps in.
What Is Regenerative Medicine?
Regenerative medicine harnesses the body’s natural healing mechanisms to repair or replace damaged tissues, including cartilage, ligaments, tendons, and even bone. These treatments aim to not only reduce symptoms but also to slow or potentially reverse the progression of arthritis.
The most promising regenerative therapies for arthritis include:
- Platelet-Rich Plasma (PRP) Therapy
- Cell-Based Therapy
- Prolotherapy
Let’s break down each of these innovative techniques.
-
Platelet-Rich Plasma (PRP) Therapy
PRP therapy involves drawing a small amount of the patient’s blood, processing it to concentrate the platelets, and then injecting this platelet-rich plasma into the affected joint.
How It Works:
Platelets contain growth factors that help stimulate tissue regeneration and reduce inflammation. When injected into an arthritic joint, PRP can:
- Promote cartilage healing
- Decrease pain and stiffness
- Improve joint function
Clinical Evidence:
Studies have shown PRP can be more effective than corticosteroids or hyaluronic acid injections in relieving knee osteoarthritis symptoms. Results are typically seen within weeks and can last for several months or even over a year.
-
Cell-Based Therapy
Stem cells are undifferentiated cells capable of transforming into various tissue types, including cartilage. In arthritis treatment, mesenchymal stem cells (MSCs) are commonly harvested from a patient’s bone marrow or adipose (fat) tissue and injected into the joint.
How It Works:
Once inside the joint, stem cells can:
- Stimulate repair of damaged cartilage
- Modulate inflammation
- Recruit other cells to aid in tissue regeneration
Clinical Evidence:
Early studies have reported significant improvements in pain, mobility, and cartilage thickness following stem cell injections. While more research is needed to establish standardized protocols, the outlook is encouraging—especially for early to moderate osteoarthritis.
-
Prolotherapy
Prolotherapy is a regenerative injection technique that involves injecting a natural irritant—often a dextrose (sugar) solution—into the joint or surrounding ligaments and tendons.
How It Works:
The solution triggers a localized inflammatory response, prompting the body to send healing cells to the area. Over time, this can strengthen connective tissues and stabilize the joint.
Who It’s For:
Prolotherapy is particularly effective for patients with joint instability, ligament laxity, or early-stage arthritis. It’s less commonly used for severe osteoarthritis but can still play a role as part of a broader regenerative plan.
Benefits of Regenerative Medicine for Arthritis
- Minimally Invasive: Most procedures are outpatient and involve little to no downtime.
- Reduced Dependence on Medications: Patients may rely less on NSAIDs, opioids, or corticosteroids.
- Slowed Disease Progression: Some therapies show the potential to halt or even reverse cartilage loss.
- Improved Quality of Life: Many patients report enhanced mobility, reduced pain, and greater participation in daily activities.
Important Considerations
Not a One-Size-Fits-All Solution
Regenerative therapies work best in the early to moderate stages of arthritis. They may not be as effective for patients with advanced joint deterioration.
Costs and Coverage
These treatments are often not covered by insurance and can range from a few hundred to several thousand dollars per session. However, many patients find the cost worthwhile for the benefits they experience.
Choose a Qualified Provider
It’s essential to seek care from physicians who specialize in regenerative medicine and follow best practices for safety, preparation, and delivery. Improper technique or unregulated products can result in complications.
The Future of Arthritis Treatment
Regenerative medicine is rapidly evolving. As research deepens and technology advances, these therapies may soon become mainstream components of arthritis care. Clinical trials are underway to determine long-term outcomes, best candidates, and optimal treatment protocols.
What’s exciting is that these approaches shift the paradigm from merely managing symptoms to actively promoting healing—a revolutionary step for the millions living with arthritis.
Final Thoughts
If you’re struggling with arthritis pain and looking for alternatives to surgery, regenerative medicine offers a promising path forward. From PRP to stem cells and beyond, these innovative techniques can help restore joint health, improve function, and reduce your reliance on medications.
Always consult a qualified healthcare professional to determine which therapy, if any, is right for you. With the right approach, living well with arthritis is not only possible—it’s becoming increasingly probable.
Interested in learning more about regenerative treatments? Talk to a regenerative medicine specialist or rheumatologist to explore your options based on your specific type of arthritis and stage of progression.
Apr 14, 2025
Joint pain can be a daily struggle, affecting everything from simple walks to sleep and overall quality of life. For many, traditional treatments like physical therapy, medications, or even surgery provide only limited relief—or come with side effects and long recovery times. That’s where regenerative medicine steps in, offering innovative options like Platelet-Rich Plasma (PRP) and Cell Therapy. These treatments harness the body’s own healing powers to target the root of joint pain, not just mask the symptoms.
If you’re curious about how PRP and Cell Therapy work, and whether they might be right for you or someone you love, read on. We’ll break down the science in simple terms and explore how these therapies are changing the way we treat joint issues.
What Causes Joint Pain?
Joint pain can stem from many sources: injury, overuse, inflammation, arthritis (especially osteoarthritis), or even simple aging. The cartilage that cushions joints can wear down, tendons and ligaments can become inflamed or torn, and the surrounding tissues may degenerate over time.
Traditionally, options like corticosteroid injections or anti-inflammatory drugs have been used to reduce pain. However, these don’t actually repair damage—they just offer temporary relief. That’s where regenerative therapies like PRP and cell therapy stand apart: they aim to stimulate healing, not just dull the pain.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a treatment that uses a concentration of your own platelets to accelerate healing in damaged joints and tissues.
How It Works:
- Blood Draw: A small amount of your blood is drawn—similar to a standard lab test.
- Separation: The blood is spun in a centrifuge to separate the platelets from other components like red and white blood cells.
- Injection: The resulting platelet-rich plasma is injected directly into the affected joint.
Platelets are best known for clotting blood, but they also contain growth factors—powerful proteins that promote tissue repair, reduce inflammation, and stimulate cell regeneration. By injecting a high concentration of these growth factors directly into the joint, PRP therapy encourages the body to repair itself.
What It’s Used For:
- Osteoarthritis (knee, hip, shoulder)
- Tendonitis
- Ligament injuries
- Cartilage damage
- Sports injuries
What Is Cell Therapy?
Cell therapy—often referred to as stem cell therapy—uses the body’s own cells to rebuild and repair damaged tissues. These aren’t embryonic stem cells but rather adult stem cells, typically derived from bone marrow or adipose (fat) tissue.
How It Works:
- Harvesting Cells: Cells are collected from your own body, usually from the bone marrow in your pelvis or fat tissue in the abdomen or thighs.
- Processing: The cells are processed and sometimes combined with PRP to enhance their effectiveness.
- Injection: The mixture is injected into the painful joint under ultrasound or fluoroscopic guidance.
These cells have the ability to differentiate—meaning they can transform into other types of cells, such as cartilage, bone, or tendon cells. They also release molecules that reduce inflammation and promote healing at the cellular level.
What It’s Used For:
- Moderate to severe osteoarthritis
- Cartilage degeneration
- Chronic joint inflammation
- Joint injuries that haven’t healed with traditional treatments
PRP vs. Cell Therapy: What’s the Difference?
| Feature |
PRP Therapy |
Cell Therapy |
| Source |
Platelets from your blood |
Stem cells from bone marrow or fat |
| Mechanism |
Stimulates healing with growth factors |
Repairs tissue by regenerating new cells |
| Best For |
Mild to moderate joint damage |
Moderate to severe degeneration |
| Invasiveness |
Minimally invasive |
Slightly more invasive (requires tissue harvesting) |
| Cost |
Lower |
Higher |
Think of PRP as a “booster” that speeds up healing, while cell therapy is a “builder” that can regenerate more extensive damage.
What to Expect from Treatment
Procedure:
Both PRP and cell therapy are usually done in an outpatient setting. The procedures typically take 1-2 hours. Since your own cells are used, the risk of allergic reactions is minimal.
Recovery:
- PRP: Mild soreness for a day or two; most people resume normal activity within 24-48 hours.
- Cell Therapy: Slightly longer recovery time due to the harvesting process; some patients may need a few days of rest.
Results:
- Most patients report a gradual reduction in pain over weeks to months.
- Improvements can last anywhere from 6 months to 2 years or more.
- Outcomes vary depending on the severity of the condition, overall health, and adherence to post-treatment guidelines like physical therapy and lifestyle changes.
The Science Behind It
PRP and cell therapy are backed by a growing body of research. For example:
- A 2020 study published in American Journal of Sports Medicine found that PRP injections significantly improved symptoms in patients with knee osteoarthritis over a 12-month period.
- A 2021 meta-analysis concluded that stem cell therapy showed consistent results in improving joint function and reducing pain in osteoarthritis patients, especially when used early in disease progression.
While not a miracle cure, these therapies are helping people delay or even avoid surgery, including joint replacement.
Is It Safe?
Yes—for most patients, PRP and cell therapy are considered safe and well-tolerated. Because the materials come from your own body, the risk of infection or rejection is extremely low. However, like any medical procedure, results aren’t guaranteed, and not everyone is a good candidate.
It’s crucial to consult with a medical provider who specializes in regenerative medicine to determine if these treatments are appropriate for your condition.
Is It Covered by Insurance?
Unfortunately, most insurance companies don’t yet cover PRP or cell therapy, viewing them as experimental. That’s slowly changing as more evidence emerges. Costs can range from a few hundred dollars (for PRP) to several thousand (for cell therapy), so be sure to ask for a cost estimate before committing.
Who’s a Good Candidate?
You might be a good candidate for PRP or cell therapy if you:
- Have chronic joint pain that hasn’t improved with rest, therapy, or medication
- Want to avoid or delay surgery
- Are in good general health
- Are not a smoker (smoking reduces healing)
- Are not severely immunocompromised or on blood thinners
The Future of Joint Pain Treatment
PRP and cell therapy offer a promising new frontier in the treatment of joint pain. These regenerative therapies don’t just cover up symptoms—they tap into the body’s natural ability to heal, rebuild, and regenerate. While they’re not a replacement for all conventional treatments, they can be a powerful tool in the journey to pain relief, better mobility, and improved quality of life.
If joint pain is holding you back, it may be time to consider a regenerative approach. Consult a knowledgeable provider to explore whether PRP or cell therapy is the right path for you.
Disclaimer: This article is for informational purposes only and should not be taken as medical advice. Always consult with a qualified healthcare provider for diagnosis and treatment recommendations.





