May 29, 2026
Chronic pain and orthopedic injuries can make everyday movement difficult, limiting activity and reducing quality of life. In recent years, regenerative medicine treatments have become increasingly popular for helping patients manage pain, promote healing, and potentially delay or avoid surgery. Treatments such as platelet-rich plasma (PRP) and other orthobiologic injections are designed to support the body’s natural healing process. However, the success of these treatments often depends on one important factor: precision.
Ultrasound-guided injections are transforming regenerative medicine by helping physicians deliver treatments more accurately. Instead of relying solely on anatomical landmarks or estimation, ultrasound technology allows healthcare providers to see muscles, tendons, ligaments, joints, and soft tissues in real time while performing an injection.
What Are Ultrasound-Guided Injections?
Ultrasound-guided injections are procedures that use live imaging technology to help physicians place needles with greater accuracy. Ultrasound creates real-time images of soft tissues, joints, tendons, nerves, and blood vessels, allowing providers to visualize exactly where the treatment is being delivered.
In regenerative medicine, precision matters because therapies are often intended to target damaged or inflamed tissue. Whether a physician is treating tendon injuries, arthritis-related pain, ligament instability, or chronic joint inflammation, accurate placement helps maximize the potential effectiveness of the treatment.
Unlike traditional “blind” injections, where providers rely on touch and anatomical landmarks, ultrasound guidance gives a clear picture beneath the skin.
Why Is Precision Important in Regenerative Treatments?
Precision is one of the most important aspects of regenerative care because many treatments are highly targeted.
For example, in platelet-rich plasma (PRP) therapy, concentrated platelets from the patient’s own blood are injected into damaged tissue to encourage healing. If the injection misses the intended target or is placed near—but not directly into—the injured structure, treatment outcomes may be less effective.
Ultrasound guidance improves precision by helping providers:
- Identify the exact area of injury or inflammation
- Avoid nearby nerves, blood vessels, and healthy tissue
- Deliver regenerative materials directly into damaged structures
- Confirm needle placement in real time
- Improve consistency and confidence during procedures
This level of accuracy can be particularly valuable in complex joints or smaller structures where precision matters most.
How Does Ultrasound Guidance Work During an Injection?
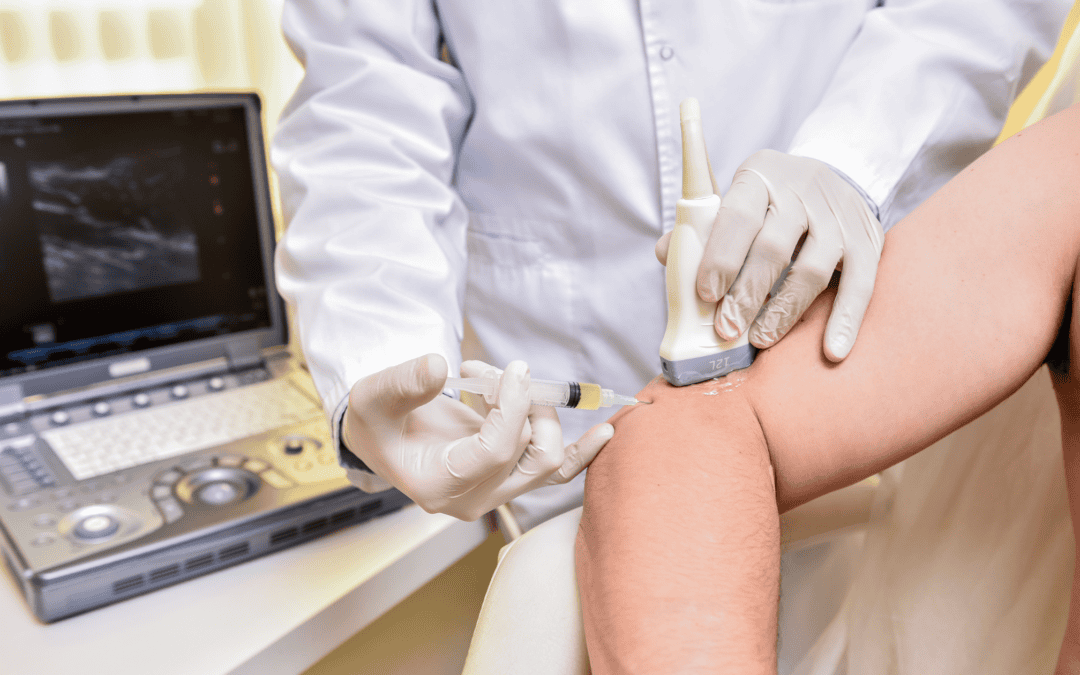
During an ultrasound-guided procedure, a provider places a handheld device called a transducer on the skin. The transducer sends sound waves into the body, which create live images on a monitor.
After locating the treatment area, the physician carefully guides the needle while watching its movement on the screen. This real-time visualization allows the provider to see both the needle and the surrounding tissues throughout the procedure.
Because ultrasound imaging happens live, physicians can make adjustments immediately if needed.
Patients are often surprised to learn that ultrasound guidance does not involve radiation. Unlike imaging technologies such as CT scans or X-rays, diagnostic ultrasound uses sound waves and is commonly used in many areas of medicine.
Which Conditions Can Benefit From Ultrasound-Guided Regenerative Injections?
Ultrasound-guided injections are commonly used for a wide range of musculoskeletal and pain-related conditions.
These may include:
Tendon Injuries
Conditions involving damaged tendons often benefit from precise regenerative injections. This can include problems such as tendon degeneration, chronic overuse injuries, or inflammation involving structures like the shoulder, elbow, knee, or ankle.
Examples include:
- Rotator cuff injuries
- Tennis elbow
- Achilles tendon injuries
- Patellar tendon problems
Arthritis and Joint Pain
Regenerative therapies may also be used for joint-related pain, particularly when arthritis affects mobility and function.
Ultrasound guidance can help target:
- Knee joints
- Hip joints
- Shoulder joints
- Small joints in the hands or feet
Greater precision may improve placement in joints where anatomy can vary from person to person.
Ligament and Soft Tissue Injuries
Ligament sprains, instability, and soft tissue damage may also benefit from image-guided regenerative treatments. Because these structures are often small and difficult to target precisely, ultrasound imaging helps providers visualize the injury location more clearly.
Chronic Pain Conditions
Certain chronic musculoskeletal pain conditions involving inflammation or tissue damage may also be treated with ultrasound-guided regenerative approaches.
The goal is often to reduce pain, improve mobility, and support long-term tissue healing.
Are Ultrasound-Guided Injections More Accurate Than Traditional Injections?
Research and clinical experience suggest that ultrasound-guided injections can improve accuracy compared to landmark-guided injections in many situations.
Without imaging guidance, even experienced providers may encounter challenges when treating smaller joints, deeper tissues, or areas with complex anatomy.
Ultrasound imaging provides several advantages:
- Real-time visualization during treatment
- Greater injection accuracy
- Reduced likelihood of missing the treatment area
- Better ability to avoid surrounding structures
- Improved confidence in needle placement
While not every procedure requires ultrasound, many specialists consider it a valuable tool for improving procedural precision.
What Should Patients Expect During the Procedure?
Most ultrasound-guided regenerative injections are performed in an outpatient setting.
The treatment area is cleaned, and ultrasound gel is applied to the skin to help produce clear images. The physician then identifies the target tissue and carefully performs the injection while monitoring the needle in real time.
Depending on the condition being treated, patients may experience mild soreness afterward. Recovery instructions vary based on the procedure and treatment area, but many people return home the same day.
Providers may recommend temporary activity modification while healing begins.
Can Ultrasound Guidance Improve Treatment Outcomes?
No medical procedure guarantees results, and outcomes vary based on the condition, severity of tissue damage, and overall patient health. However, greater accuracy may improve the ability to place regenerative treatments where they are intended to work.
Because regenerative medicine focuses on targeted healing, many physicians view precision as an important factor in maximizing potential benefits.
For patients considering regenerative care, asking whether ultrasound guidance is used during treatment may be an important part of understanding the overall approach.
Final Thoughts
Ultrasound-guided injections are helping improve precision in regenerative medicine by allowing physicians to see tissues and guide treatment in real time. Whether treating tendon injuries, joint pain, arthritis, or soft tissue problems, accurate placement may help support better-targeted care.
As regenerative medicine continues to evolve, ultrasound guidance is becoming an increasingly valuable tool for improving confidence, accuracy, and personalized treatment planning. Patients exploring non-surgical options for chronic pain or orthopedic injuries may benefit from discussing image-guided regenerative treatments with a qualified provider.
May 21, 2026
Chronic tendon injuries can make everyday activities difficult and frustrating. Whether it is persistent shoulder pain, tennis elbow, Achilles tendinopathy, or chronic knee tendon irritation, these conditions often linger for months or even years. Traditional treatment options like rest, physical therapy, anti-inflammatory medications, or surgery do not always provide complete relief.
Today, advances in regenerative medicine are changing how chronic tendon injuries are treated. Orthobiologics are emerging as a promising option for patients seeking to reduce pain, improve function, and potentially avoid surgery.
What Are Chronic Tendon Injuries?
Tendons connect muscles to bones and help create movement throughout the body. Over time, repetitive stress, overuse, aging, or poor healing can cause tendon tissue to break down. This process is often referred to as tendinopathy or tendinosis rather than simple inflammation.
Common chronic tendon injuries include:
- Rotator cuff tendinopathy in the shoulder
- Tennis elbow (lateral epicondylitis)
- Golfer’s elbow
- Patellar tendinopathy (“jumper’s knee”)
- Achilles tendinopathy
- Hamstring tendon injuries
Unlike acute injuries, chronic tendon problems often involve degeneration of the tendon tissue rather than active inflammation. This is one reason why treatments like anti-inflammatory medications may only provide temporary symptom relief.
What Are Orthobiologics?
Orthobiologics are biologic substances used to help support the body’s natural healing process. These treatments are commonly derived from the patient’s own blood, bone marrow, or tissue and are designed to encourage tissue repair and regeneration.
Orthobiologic treatments commonly used for tendon injuries include:
- Platelet-rich plasma (PRP)
- Bone marrow aspirate concentrate (BMAC)
- Mesenchymal stem cell-based therapies
Research into orthobiologics continues to expand as physicians look for minimally invasive alternatives to surgery for musculoskeletal conditions.
Platelet-Rich Plasma (PRP) for Tendon Healing
PRP remains one of the most widely used orthobiologic treatments for chronic tendon injuries.
PRP is created by drawing a patient’s blood and processing it to concentrate platelets and growth factors. The PRP is then injected directly into the injured tendon under ultrasound guidance.
These growth factors may help:
- Stimulate tissue repair
- Improve blood flow
- Support collagen production
- Reduce pain
- Promote a healthier healing environment
PRP has been studied in conditions such as tennis elbow, Achilles tendinopathy, and rotator cuff disease. While results can vary depending on the condition and severity of injury, many patients experience improved pain and function after treatment.
One of the newer areas of research involves optimizing PRP formulations. Physicians are now studying differences between leukocyte-rich and leukocyte-poor PRP to determine which may work best for specific tendon conditions.
Bone Marrow Aspirate Concentrate (BMAC)
BMAC is another advanced orthobiologic option gaining attention for chronic tendon injuries.
This treatment involves collecting bone marrow—typically from the pelvis—and concentrating it to isolate healing cells, growth factors, and signaling proteins. The concentrated material is then injected into the damaged tendon.
BMAC may provide a more robust regenerative environment compared to traditional injections because it contains:
- Mesenchymal stem cells
- Cytokines
- Growth factors
- Anti-inflammatory signaling molecules
Emerging evidence suggests BMAC may be beneficial for more severe or long-standing tendon degeneration.
Can Orthobiologics Help Patients Avoid Surgery?
For some patients, orthobiologic treatments may help reduce pain and improve function enough to delay or avoid surgery. This is especially appealing for individuals who:
- Have chronic tendon pain despite conservative treatment
- Want to remain active
- Prefer minimally invasive options
- Are not ideal surgical candidates
- Want to support healing without prolonged downtime
However, orthobiologics are not a cure-all solution. Outcomes vary depending on:
- The severity of tendon damage
- Overall health
- Activity level
- The specific biologic treatment used
- Rehabilitation after treatment
In some cases, surgery may still be necessary, particularly for complete tendon tears or advanced structural damage.
The Importance of Proper Diagnosis and Rehabilitation
Successful treatment of chronic tendon injuries requires more than injections alone. A comprehensive treatment plan often includes:
- Diagnostic ultrasound or MRI evaluation
- Physical therapy
- Strengthening and mobility work
- Activity modification
- Biomechanical correction
- Guided rehabilitation
Orthobiologic treatments are often most effective when combined with a carefully designed recovery program that supports long-term tendon healing.
The Future of Tendon Injury Treatment
The field of orthobiologics continues to advance as research expands and regenerative therapies become more refined. While not every patient will require these treatments, orthobiologics are creating new possibilities for people living with chronic tendon pain who want alternatives beyond surgery and long recovery periods.
As technology and clinical evidence continue to evolve, regenerative medicine may play an increasingly important role in helping patients restore mobility, reduce pain, and return to the activities they enjoy.
Apr 24, 2026
Joint pain and cartilage damage can significantly impact your daily life, making simple movements uncomfortable or even debilitating. While traditional treatments like medications, injections, or surgery can offer relief, many patients are now turning to regenerative medicine for a more natural and long-lasting solution. One of the most promising options is LIPOGEMS® Microfragmented Fat Therapy.
This innovative treatment uses your body’s own fat tissue to help repair and support damaged joints and cartilage—without the need for major surgery.
What Is LIPOGEMS® Microfragmented Fat Therapy?
LIPOGEMS® is a minimally invasive procedure that involves harvesting a small amount of fat (adipose tissue) from your body—typically from the abdomen or thighs—and processing it into a purified, microfragmented form.
This processed fat is rich in:
- Mesenchymal stem cells (MSCs)
- Growth factors
- Anti-inflammatory signaling molecules
Once prepared, the microfragmented fat is injected directly into the affected joint or damaged area to promote healing and tissue regeneration.
How Does It Work?
The effectiveness of LIPOGEMS® therapy comes from its ability to harness the natural healing properties of your own body.
1. Reduces Inflammation
Chronic inflammation is a major contributor to joint pain and cartilage breakdown. The bioactive components in microfragmented fat help modulate the inflammatory response, creating a healthier environment for healing.
2. Promotes Tissue Repair
The stem cells and growth factors within the fat tissue support the repair of damaged cartilage and surrounding structures. While it may not fully regenerate cartilage in advanced cases, it can significantly improve joint function and slow further degeneration.
3. Improves Joint Lubrication
LIPOGEMS® injections can enhance the joint environment, helping improve lubrication and reduce friction—leading to smoother, less painful movement.
4. Supports Long-Term Healing
Unlike temporary treatments that mask pain, this therapy works at a cellular level to promote ongoing healing over time.
What Conditions Can It Help Treat?
LIPOGEMS® Microfragmented Fat Therapy is commonly used for a variety of orthopedic conditions, including:
- Knee osteoarthritis
- Hip arthritis
- Shoulder injuries
- Meniscus tears
- Ligament and tendon injuries
- Early cartilage damage
It is particularly beneficial for patients who want to delay or avoid joint replacement surgery.
What to Expect During the Procedure
The LIPOGEMS® procedure is typically performed in an outpatient setting and involves three main steps:
- Fat Harvesting – A small amount of fat is collected using a gentle liposuction technique.
- Processing – The fat is purified and microfragmented using a specialized system without chemicals or additives.
- Injection – The processed tissue is injected into the targeted joint using imaging guidance for precision.
The entire process usually takes about one to two hours.
Recovery and Results
Recovery from LIPOGEMS® therapy is generally quick and well-tolerated:
- Mild soreness or swelling may occur at the harvest or injection site
- Most patients return to normal activities within a few days
- Improvement is often gradual, with results developing over several weeks to months
Many patients report reduced pain, improved mobility, and enhanced quality of life.
Is LIPOGEMS® Right for You?
LIPOGEMS® therapy may be a good option if you:
- Have mild to moderate joint degeneration
- Want to avoid or delay surgery
- Have not found relief with traditional treatments
- Are looking for a natural, regenerative approach
However, it may not be suitable for severe joint damage or advanced arthritis. A thorough evaluation by a pain management or orthopedic specialist is essential to determine if this treatment is appropriate for you.
Final Thoughts
LIPOGEMS® Microfragmented Fat Therapy represents an exciting advancement in regenerative medicine. By using your body’s own healing potential, this treatment offers a minimally invasive way to reduce pain, improve joint function, and support cartilage health.
If you’re struggling with joint pain and looking for alternatives to surgery, LIPOGEMS® may provide the relief and recovery you’ve been searching for.
Apr 9, 2026
Chronic joint and tendon pain can significantly impact your quality of life—limiting movement, reducing activity levels, and making even everyday tasks uncomfortable. While traditional treatments like medications, physical therapy, and surgery have long been the standard, regenerative medicine is transforming how we approach musculoskeletal injuries. One of the most promising advancements in this space is Platelet-Rich Plasma (PRP) therapy.
PRP therapy offers a minimally invasive, non-surgical option that uses your body’s natural healing mechanisms to repair damaged tissues. But what exactly is PRP, and how does it work? Let’s break it down.
What Is PRP Therapy?
Platelet-Rich Plasma (PRP) therapy is a regenerative treatment that uses a concentrated form of your own blood to promote healing. Blood contains several components, including red blood cells, white blood cells, plasma, and platelets. Platelets are especially important because they contain growth factors and proteins that play a key role in tissue repair and regeneration.
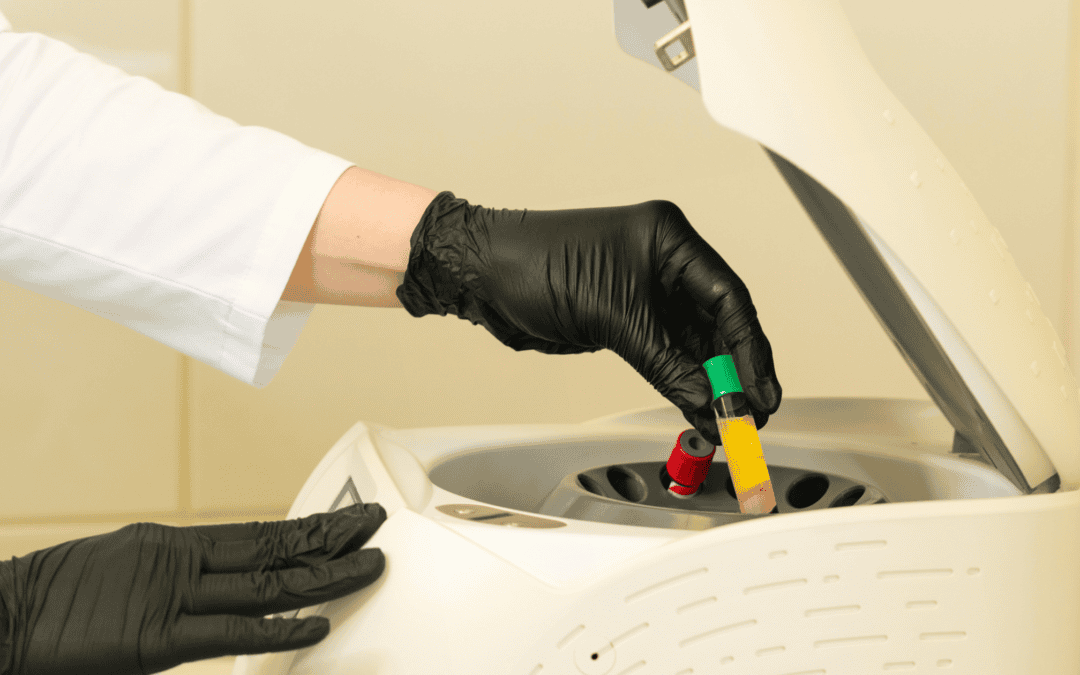
In PRP therapy, a small sample of your blood is drawn and placed in a centrifuge. This process separates the platelets from other blood components, creating a concentrated solution rich in healing factors. The PRP is then injected directly into the injured or painful area.
How PRP Promotes Healing
- Stimulates cell regeneration
- Promotes collagen production
- Improves blood flow to the injured area
- Reduces inflammation
- Accelerates tissue repair
Unlike corticosteroid injections, which primarily reduce inflammation temporarily, PRP targets the underlying cause of pain by supporting actual tissue healing.
Conditions PRP Can Treat
Joint Conditions
- Osteoarthritis (knee, hip, shoulder)
- Degenerative joint disease
- Cartilage injuries
Tendon Injuries
- Tennis elbow (lateral epicondylitis)
- Golfer’s elbow (medial epicondylitis)
- Achilles tendinitis
- Patellar tendinitis (jumper’s knee)
- Rotator cuff injuries
Ligament Injuries
- Partial ligament tears
- Chronic sprains
What to Expect During the Procedure
- Blood Draw: A small amount of blood is taken from your arm.
- Centrifugation: The blood is spun in a centrifuge to isolate the platelet-rich plasma.
- Injection: The PRP is injected into the targeted area, often using ultrasound guidance for precision.
Recovery and Results
One of the major advantages of PRP therapy is its relatively quick recovery time. Because it is a minimally invasive procedure, patients can often return to normal activities within a few days.
However, it’s important to note that PRP is not an instant fix. Since it works by stimulating natural healing, results develop gradually over time. Patients may begin to notice improvement within a few weeks, with continued progress over several months.
Benefits of PRP Therapy
- Minimally invasive
- Uses your body’s own cells
- Targets the root cause of pain
- Reduced downtime
- Versatile treatment option
Are You a Good Candidate for PRP?
PRP therapy is an excellent option for many patients, but it may not be suitable for everyone. Ideal candidates typically include individuals who have chronic joint or tendon pain, have not found relief with conservative treatments, and want to avoid or delay surgery.
PRP vs. Other Treatments
Corticosteroid injections provide short-term relief but do not promote healing. Physical therapy is beneficial but may not be enough for chronic conditions. Surgery can be effective but comes with higher risks and longer recovery times. PRP offers a regenerative alternative without the invasiveness of surgery.
Final Thoughts
If you’re struggling with persistent joint or tendon pain, PRP therapy may offer a safe, effective, and minimally invasive solution. By harnessing your body’s natural healing power, this innovative treatment helps restore function and improve quality of life.
At SDOMG, our team specializes in advanced, patient-centered treatments designed to help you get back to the activities you love. Schedule a consultation today to learn if PRP therapy is right for you.
Mar 20, 2026
Chronic pain is rarely caused by a single issue—and it rarely responds to a one-size-fits-all solution. For many patients, long-term relief requires a comprehensive, personalized approach that addresses both symptoms and underlying causes. One of the most promising additions to modern pain management is regenerative medicine.
Rather than simply masking discomfort, regenerative therapies aim to support the body’s natural healing processes. When combined with other treatments, regenerative medicine can play a powerful role in reducing pain, improving function, and enhancing overall quality of life.
What Is Regenerative Medicine?
Regenerative medicine focuses on repairing or restoring damaged tissues using the body’s own biological resources. Two of the most commonly used treatments in pain management include:
- Platelet-Rich Plasma (PRP): A concentration of platelets derived from your own blood, rich in growth factors that promote healing.
- Stem Cell Therapy: Uses specialized cells (often from bone marrow or adipose tissue) that can help repair damaged structures and reduce inflammation.
These therapies are often used to treat conditions involving joints, ligaments, tendons, and even certain spinal issues.
Why Regenerative Medicine Matters in Pain Care
Traditional pain treatments—such as medications, injections, or even surgery—often focus on symptom control. While these approaches can be effective, they don’t always address the root cause of the problem.
Regenerative medicine offers a different approach by:
- Supporting tissue repair and healing
- Reducing inflammation at the source
- Potentially delaying or avoiding surgery
- Promoting longer-lasting relief compared to temporary treatments
Conditions Commonly Treated with Regenerative Therapies
Regenerative medicine is frequently used as part of a broader pain management strategy for conditions such as:
- Osteoarthritis (knee, hip, shoulder)
- Tendon injuries (such as rotator cuff or Achilles tendon issues)
- Ligament sprains and instability
- Degenerative disc disease
- Chronic joint pain
Integrating Regenerative Medicine into a Comprehensive Plan
The most effective pain management strategies combine multiple therapies tailored to the individual. Regenerative medicine is rarely used in isolation—instead, it works best as part of a coordinated plan that may include:
Physical Therapy
Rehabilitation helps strengthen surrounding muscles, improve mobility, and support healing after regenerative treatments.
Interventional Procedures
Targeted injections, nerve blocks, or minimally invasive procedures can provide additional pain relief and improve function.
Lifestyle Modifications
Weight management, nutrition, posture, and activity adjustments all play a role in long-term success.
Behavioral and Psychological Support
Chronic pain affects both the body and mind. Stress management, cognitive behavioral therapy, and sleep optimization can enhance treatment outcomes.
What to Expect from Treatment
Regenerative therapies are typically performed in an outpatient setting and involve minimal downtime. However, results are not immediate. Because these treatments stimulate natural healing, improvement often occurs gradually over weeks to months.
Patients may experience:
- Mild soreness after the procedure
- Gradual reduction in pain
- Improved strength and function over time
A series of treatments may be recommended depending on the condition and severity.
Is Regenerative Medicine Right for You?
Regenerative medicine is an exciting and evolving field, but it is not a cure-all. The best candidates are typically individuals who:
- Have chronic musculoskeletal pain
- Want to avoid or delay surgery
- Have not found sufficient relief from conservative treatments
- Are committed to a comprehensive care plan
A thorough evaluation by a qualified pain specialist is essential to determine whether these therapies are appropriate.
The Bottom Line
Regenerative medicine represents a shift in how we approach pain care—from simply managing symptoms to actively supporting healing. When integrated into a comprehensive treatment plan, therapies like PRP and stem cell injections can help patients achieve meaningful, lasting improvements.
If you are living with chronic pain, exploring regenerative options as part of a broader strategy may open the door to better outcomes and a more active, comfortable life.

Jan 23, 2026
Platelet-rich plasma (PRP) injections have gained attention as a regenerative treatment option for patients seeking relief from joint, tendon, ligament, and soft tissue pain. Often used in orthopedics, sports medicine, and pain management, PRP offers a minimally invasive approach designed to support the body’s natural healing processes. If you’re considering PRP therapy, understanding how it works, what it treats, and what to expect can help you make an informed decision.
What Are PRP Injections?
PRP stands for platelet-rich plasma. Platelets are a natural component of blood best known for their role in clotting, but they also contain growth factors that support tissue repair.
During a PRP procedure:
- A small amount of the patient’s blood is drawn
- The blood is spun in a centrifuge to concentrate the platelets
- The platelet-rich portion is injected into the targeted area
Because PRP is derived from the patient’s own blood, the risk of allergic reaction or rejection is extremely low.
How PRP Supports Healing
PRP works by delivering a high concentration of growth factors directly to injured or degenerative tissue. These growth factors may:
- Promote tissue repair
- Reduce inflammation
- Support collagen production
- Encourage cellular regeneration
Rather than simply masking pain, PRP aims to improve the underlying tissue environment to support longer-term healing.
Conditions Commonly Treated with PRP
PRP injections may be recommended for a variety of musculoskeletal conditions, including:
- Knee, hip, and shoulder osteoarthritis
- Tendon injuries (such as tennis elbow or Achilles tendinopathy)
- Ligament sprains
- Chronic joint pain
- Muscle injuries
- Certain spine-related soft tissue conditions
PRP is often considered when conservative treatments like physical therapy or medications have not provided sufficient relief.
What to Expect During and After Treatment
PRP injections are typically performed in an outpatient setting and usually take less than an hour.
After the procedure:
- Mild soreness or swelling at the injection site is common
- Patients are often advised to limit strenuous activity for several days
- Pain relief and functional improvement may develop gradually over weeks
Because PRP stimulates a biological healing response, results are not immediate. Some patients may require a series of injections depending on the condition being treated.
Is PRP Right for Everyone?
While PRP is generally safe, it may not be appropriate for all patients. Factors such as:
- Severity of tissue damage
- Overall health
- Blood disorders or active infections
- Treatment goals
should be discussed with a qualified medical provider. PRP is not a replacement for surgery in severe structural damage, but it may help delay or reduce the need for more invasive procedures.
It’s also important to note that PRP is considered a biologic therapy, and coverage varies because it is not universally approved by U.S. Food and Drug Administration for all indications.
PRP vs. Steroid Injections
Unlike corticosteroid injections, which primarily reduce inflammation and pain temporarily, PRP aims to support tissue repair. Steroids may provide faster relief but can weaken tissues with repeated use. PRP may take longer to show results but is often chosen for its regenerative potential.
Final Thoughts
PRP injections represent an evolving approach in regenerative and pain medicine, offering patients a minimally invasive option that works with the body’s natural healing abilities. While results vary, many patients find PRP to be a valuable part of a comprehensive, non-surgical treatment plan.
If you’re experiencing ongoing joint or soft tissue pain, a consultation with a pain management or regenerative medicine specialist can help determine whether PRP is an appropriate option for you.





